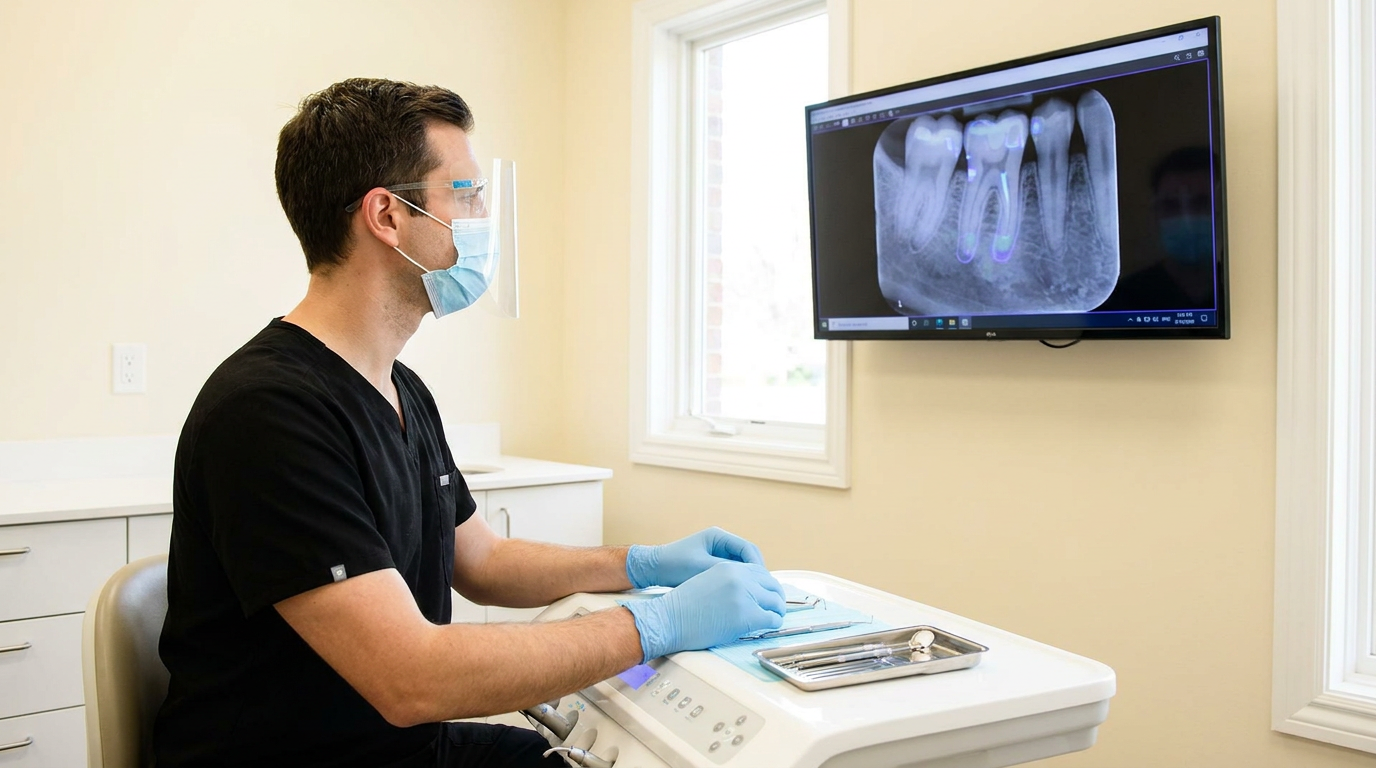
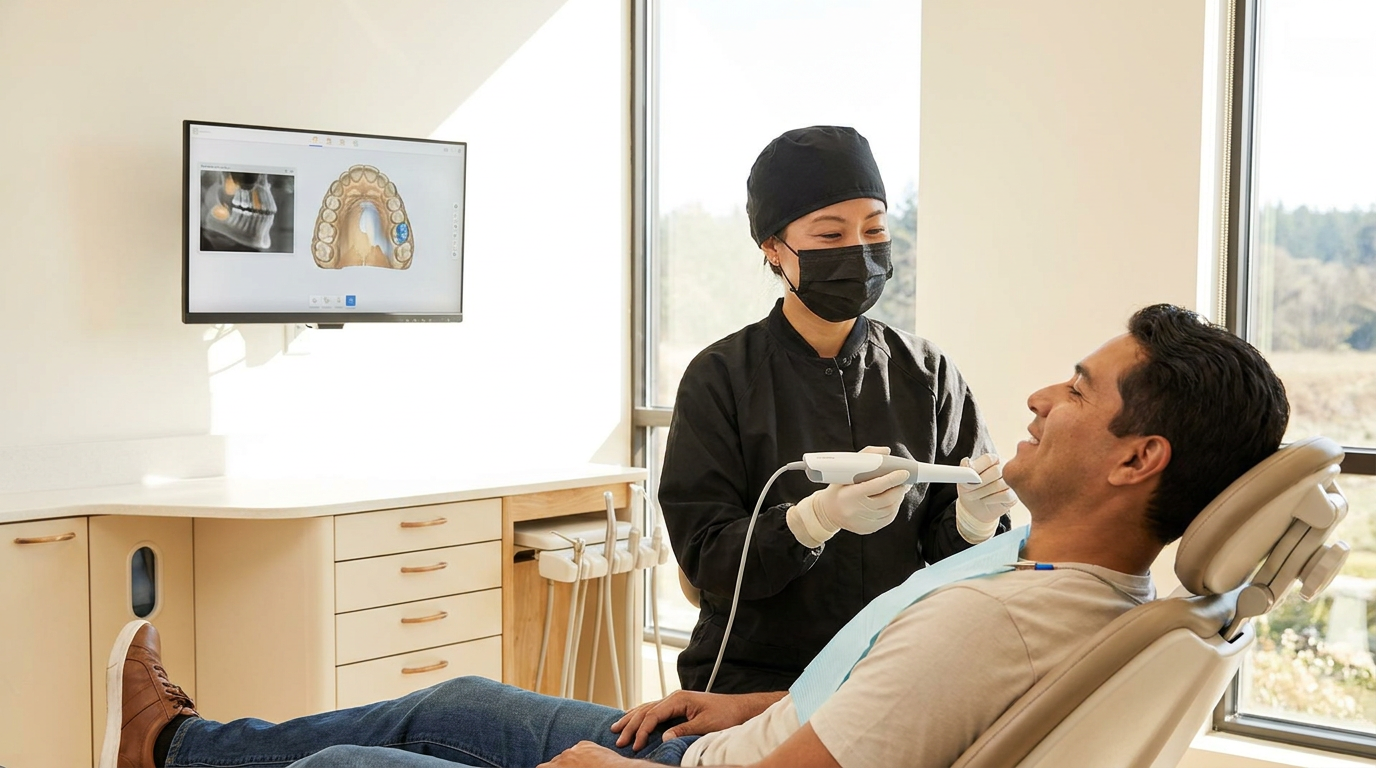
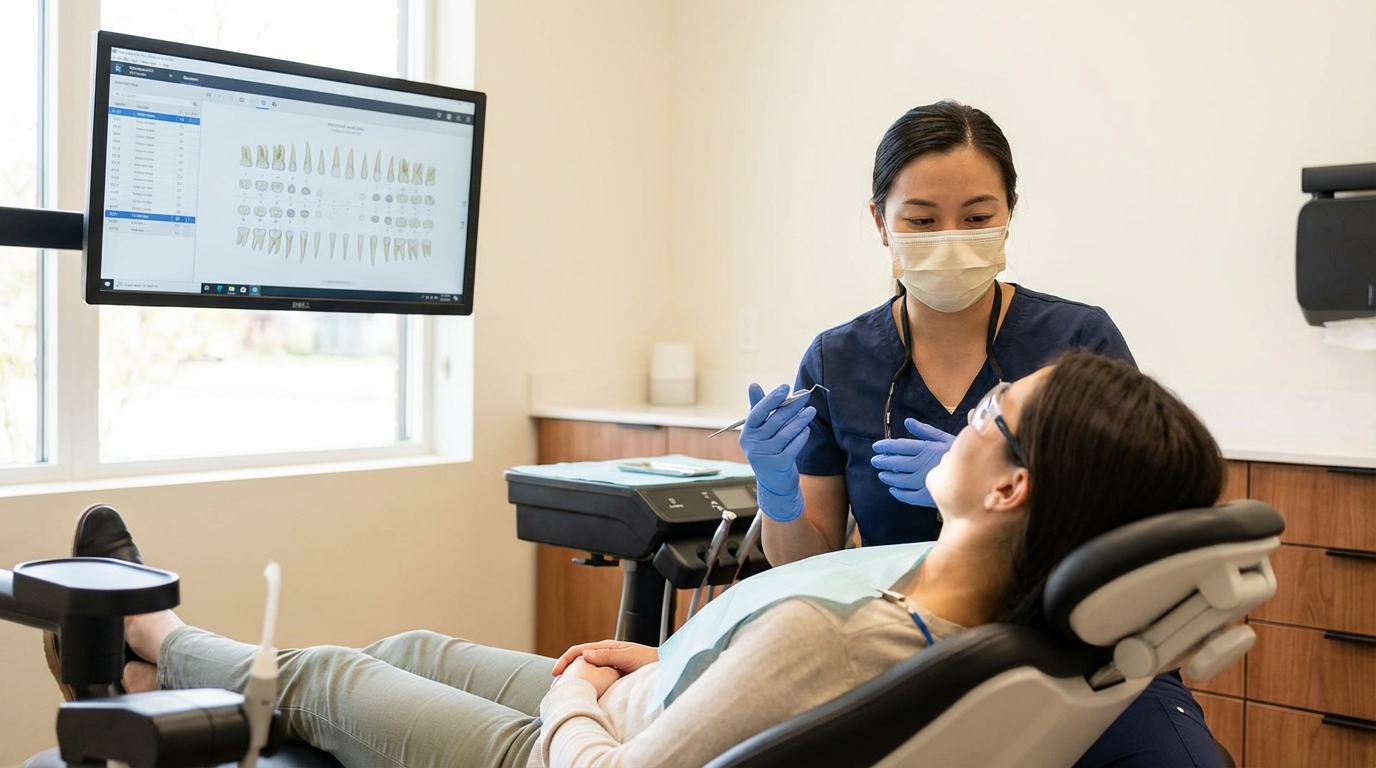
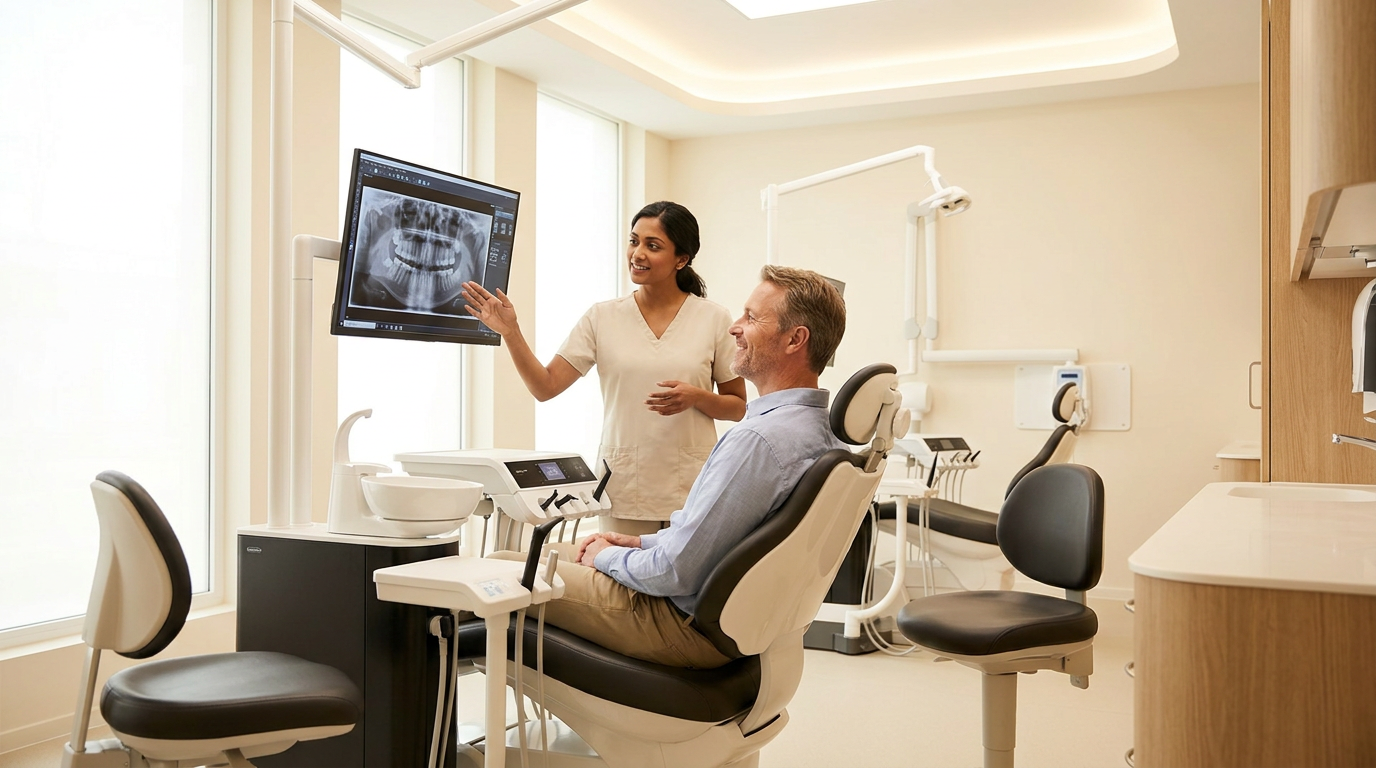
Diagnostic inconsistency across your network isn't a people problem, it is a reference point problem, and the fix doesn't require a mandate.
Pull chart audits across ten locations and you will find ten different diagnostic thresholds for the same clinical conditions. Not because your dentists are careless. Because clinical judgment, operating without a shared baseline, naturally drifts over time. Every provider brings their training, their pattern recognition, their tolerance for ambiguity, and none of that is wrong in isolation. The problem is that it produces different answers for the same radiographic presentation depending on which chair the patient sits in. You know what that costs operationally. The harder question is how to correct it without your providers reading the correction as an audit of their clinical judgment, and without losing the trust you've spent years building with the clinicians who make your network run.
Why Diagnostic Drift Is Structural and What It's Costing Your Network
Diagnostic inconsistency produces three downstream consequences that compound each other.
The first is chart disputes. When providers reach different findings on comparable presentations, chart reviews generate rework. That rework erodes provider trust in the review process itself, which makes future quality conversations harder to have. Providers who feel their documentation is being second-guessed become defensive, and defensive providers stop engaging with quality programs.
The second is payor exposure. Treatment plans built on variable diagnostic thresholds do not hold up uniformly under payor scrutiny. When charts lack the objective clinical documentation to support the treatment recorded, you get audit friction, claim denials, and the administrative drag that follows. The provider who wrote the chart experiences that friction directly, as a challenge to their clinical defensibility, not as an organizational problem.
The third is patient inconsistency. A patient who visits two locations in your network and receives materially different diagnoses for the same condition does not conclude that dentistry is complex. They conclude that your organization does not have a standard of care. That perception compounds over time and it travels.
The Diagnostic Reference Point That Changes the Equation
The DSOs that have solved diagnostic inconsistency at scale have not done it by writing better clinical policies or running more training sessions. They have done it by giving every provider access to the same objective clinical baseline before any treatment decision is made.
The clinical credibility foundation for this kind of standardization already exists. Overjet products are backed by 11 FDA clearances, more than any other dental AI company.
FDA clearance is a regulatory designation, not a marketing claim. It places Overjet in the same category as the diagnostic instruments your providers already use without debate, not in the category of corporate tools that require internal selling. When a provider asks whether the evidence is strong enough, the answer is not your opinion. It is a federal regulatory standard.
The credibility burden shifts from you to the regulatory body, and that is the only shift that works with senior clinicians who will push back on anything that sounds like a corporate initiative.
The Evidence Behind the Playbook and the Adoption Architecture That Makes It Stick
The most common worry clinical leaders have is that standardization means mandate, that you are replacing clinical judgment with a corporate checklist. Overjet surfaces objective findings, the dentist still decides what to do with them. Standardization removes diagnostic ambiguity. It does not remove clinical autonomy.
The clinical validation supports this framing. One hundred percent of dentists who used the tool found more caries. Not most, not a strong majority: all of them. Ninety-one percent found more periodontal disease. The diagnostic lift spans the full scope of conditions that create concordance risk across locations. Every dentist who used it found more. That is a peer-validation signal, not a performance claim, and it is the specific, citable data point you can use in a hallway conversation with a skeptical senior clinician.
The rollout that works is peer-led. You do not announce the tool network-wide. You identify two or three clinically respected early adopters, run a structured pilot with clear KPI tracking, and let their outcomes carry the internal conversation. Senior clinicians are not the obstacle in this model. They are the channel. The framing that works in that conversation: "I'm recommending this because it makes you a better dentist, not because I have to."
Providers who expected workflow friction found the opposite. The tool integrates into existing exam workflow and reduces the documentation burden that follows ambiguous findings. The clinical burden is lower, not higher.
The outcome metrics close the loop. Case acceptance increases 25% with AI-assisted diagnostics. Treatment acceptance lifts 15 to 25% with AI-assisted visualization. Dental groups using this approach see an average 10x ROI, driven by production gains that do not require additional chair time or headcount. That is the number you will need when this conversation moves to the CFO.
What's Next
Diagnostic standardization across locations is not a mandate problem. It is a reference point problem, and the reference point now exists in a clinically validated, FDA-cleared form that providers will trust because it is proven, not because they were told to.
Schedule a call to see how Overjet's diagnostic standardization framework is being deployed across DSO networks and what a pilot rollout could look like for your organization.
The CCO who builds this playbook does not just solve an audit problem. They become the clinical leader whose providers say the tool made them better dentists.
Here's What CCOs Ask Us Most
How do I measure whether diagnostic standardization is actually working across my locations?
Track three KPIs: diagnostic concordance rate, treatment acceptance rate, and audit pass rate. Concordance tells you whether providers are reaching consistent findings on comparable radiographic presentations. Acceptance tells you whether patients are saying yes at consistent rates across locations. Audit pass rate tells you whether charts are holding up under payor review without dispute. If concordance is rising and acceptance is rising, the playbook is working.
Is the clinical evidence strong enough that my dentists will actually trust this, or will they push back on it as a corporate initiative?
The credibility foundation is FDA clearance. Overjet is the only AI platform cleared by the FDA for both caries detection and bone level quantification. That is a regulatory designation, not a marketing claim, and it is the same standard providers apply to every other diagnostic instrument in their operatory. The internal conversation shifts when providers understand they are not being asked to trust a corporate tool. They are being asked to use a clinically validated instrument that has already passed federal regulatory review.
What does a realistic rollout look like for a network our size, and how do I avoid a network-wide resistance event?
The rollout that works is peer-led, not top-down. Identify two or three clinically respected early adopters, run a structured pilot with clear KPI tracking, and let their outcomes carry the internal conversation. You do not announce the tool. You let the results announce it. Senior clinicians are not the obstacle in this model. They are the distribution channel.
Will this tool slow down my exams or add more documentation work to my day?
Providers consistently report the opposite. The tool reduces documentation burden by surfacing objective findings that are already defensible, which eliminates the time spent qualifying ambiguous chart notes after the fact. Providers who expected friction found that the tool integrates into existing exam workflow without adding a new system layer. The clinical burden is lower, not higher, and 100% of dentists who used it found more caries, which means the cases they were already seeing became more complete, not more complicated.
What is the downstream financial case if I need to bring this to my CFO or COO?
Dental groups using AI-assisted diagnostic standardization see an average 10x ROI, driven primarily by case acceptance lift. A 25% increase in case acceptance translates directly into production per practice without adding chair time or headcount. The clinical case closes the CCO. The ROI number closes the CFO. You will need both, and the data supports both.