The Cost Model Looks Clean Until It Doesn't
Every dental software vendor hands you a TCO spreadsheet that works perfectly under their assumptions. Adoption hits 90% on day 60. Implementation wraps in four weeks. Support fees stay flat across 50 locations. Those assumptions are not your numbers, and when they break, the payback period doubles.
The cost categories that determine whether a dental AI investment pays back in 12 months or 36 are rarely in the proposal: change-management labor, per-location implementation overruns, and the revenue drag from providers who were trained but never adopted the workflow.
What the Standard TCO Model Omits
Vendor TCO models are built around license fees and projected production uplift. The categories that compound after signature are the ones left off the line items.
Clinical adoption is the variable most likely to invalidate a TCO model. A platform that 40% of providers use consistently produces a fraction of the projected revenue impact, but the license fee is the same. Most vendor models present adoption as a given, not a risk with a cost.
Implementation overruns are the second omission. Per-location implementation cost is predictable in a pilot and unpredictable at scale if the vendor has no mechanism to track it in real time. At 20 locations, a 15% overrun per site is a material budget variance.
Support fees that compound across a growing location count are the third. Contracts that do not cap migration and support costs create an open liability that grows with the DSO.
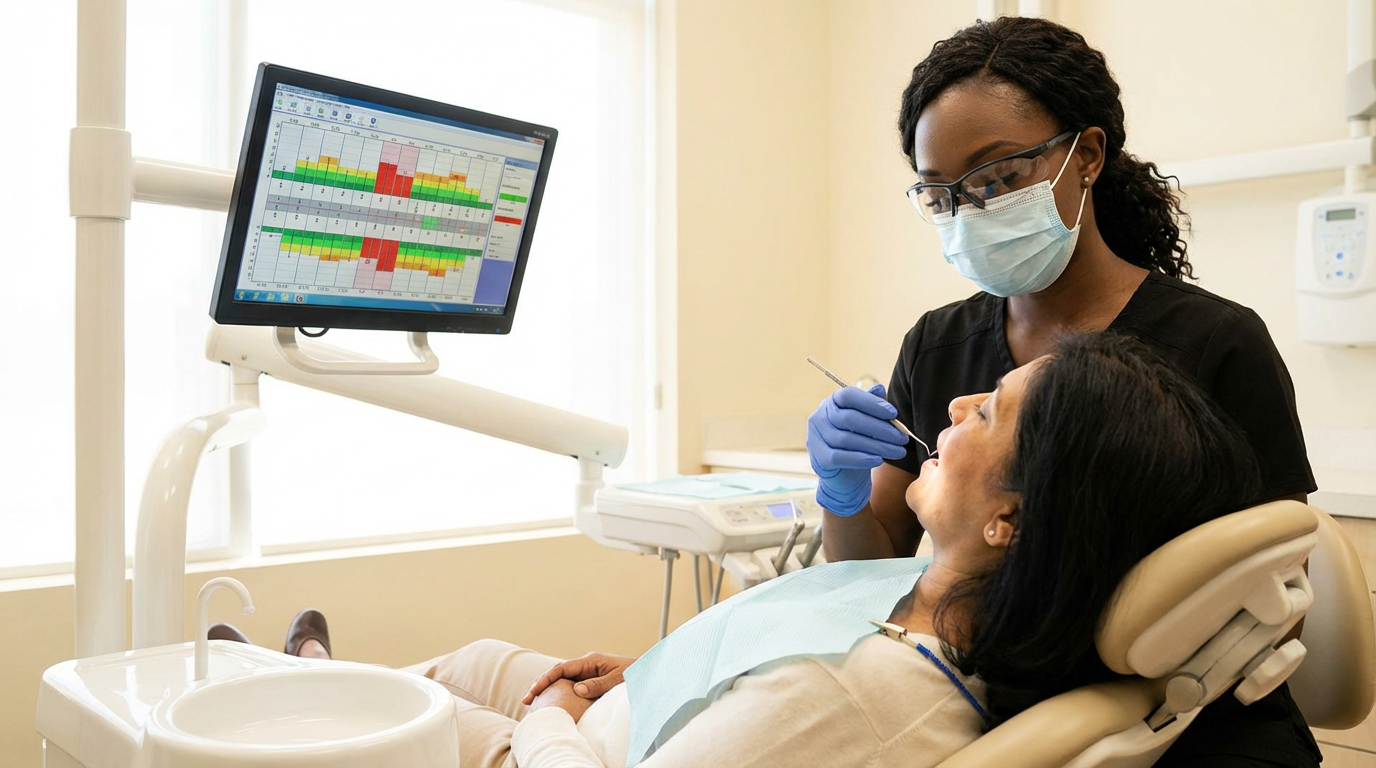
Perio screening inconsistency suppresses hygiene production at every location where a case goes undetected. That revenue loss does not appear in a vendor's TCO model, but it is a direct cost of not standardizing the diagnostic workflow.
A complete TCO model for dental AI covers four line items across a three-year horizon: per-location implementation cost tracked against budget, adoption rate by provider and location, revenue impact per practice measured against baseline, and support and migration fees capped by contract.
Building the Model on Your Numbers
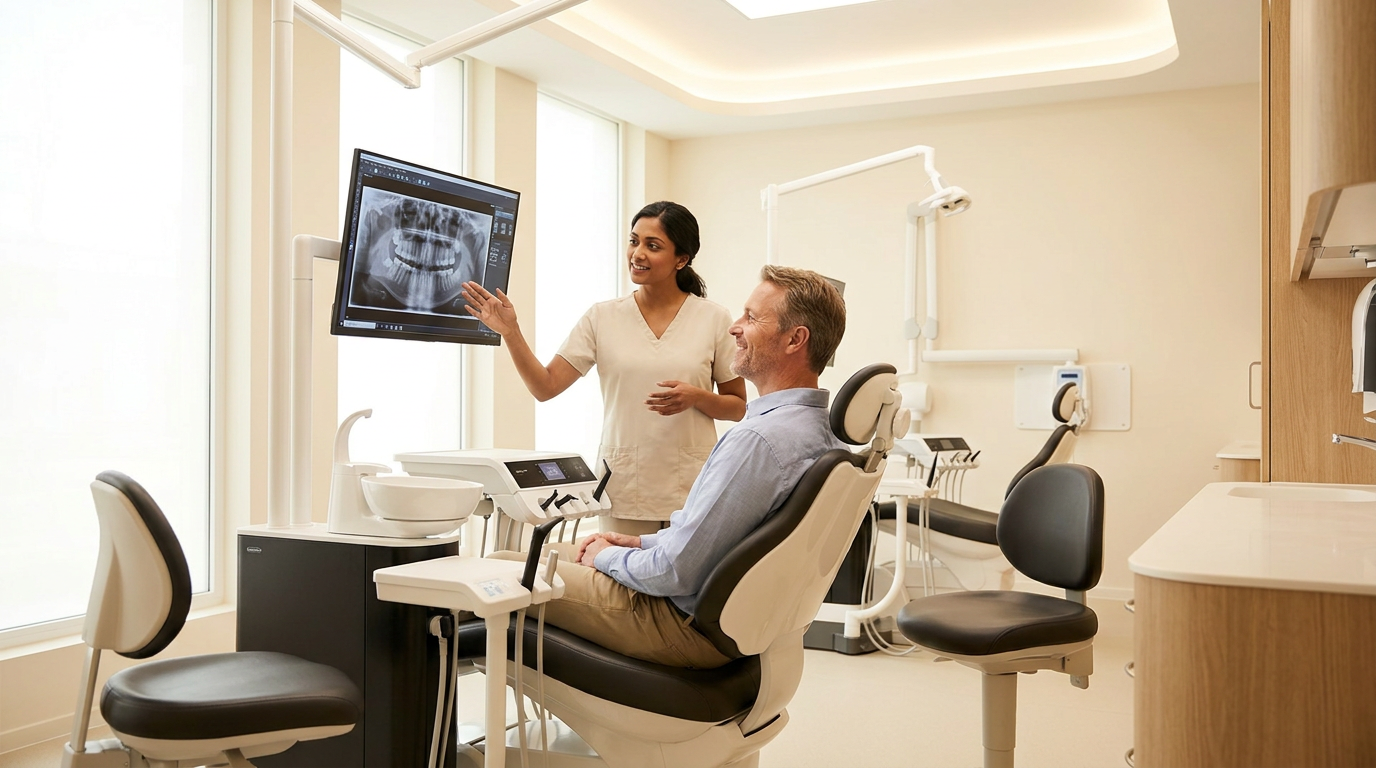
Overjet holds 10 FDA clearances, including caries detection and bone level quantification, more than any other dental AI company. Those clearances are the clinical credibility foundation that accelerates provider adoption, because dentists are working with a standard that has passed FDA scrutiny for the specific findings they document and bill.
Faster provider adoption reduces the change-management cost in the TCO model. It also shortens the months-to-payback calculation, because production uplift begins earlier in the deployment timeline.
Overjet's pilot-first structure runs 3 to 5 locations before any full rollout commitment. The pilot produces measured production-per-practice data, adoption rates, and implementation cost actuals from your own locations. Those are your numbers, and they are the numbers you take to a board or PE sponsor to defend the rollout budget.
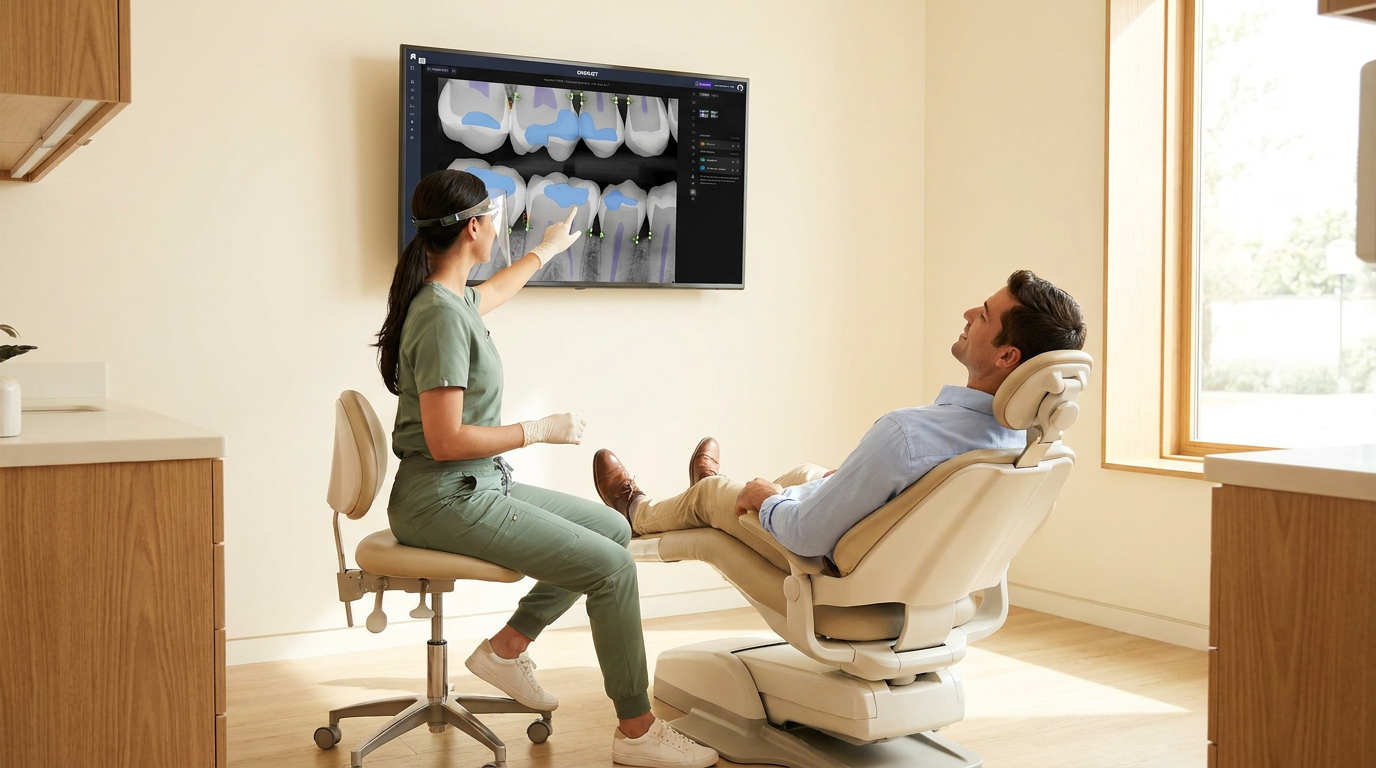
Overjet produces a 15-to-25% increase in treatment acceptance with AI-assisted visualization. Modeled against per-location implementation cost from the pilot, that uplift produces a payback period you can calculate before committing rollout budget.
Managing Adoption Risk and Utilization
Adoption risk is the variable that determines whether the payback period holds or extends. Overjet tracks utilization daily and intervenes the same day when adoption drops at a location. Adoption problems are corrected in real time, not discovered at a quarterly business review when three months of projected revenue have already been missed.
Claims velocity compounds the financial return. Overjet produces 5x faster claims decisions, which accelerates cash flow across all locations and reduces the working capital drag that slow revenue cycles create in a multi-location DSO. That impact is additive to the production uplift number.
The financial benchmark for dental groups using Overjet is a 10x average ROI. That number gives you a peer reference point to stress-test the vendor's projections before committing rollout budget. If your model produces a materially lower return at current adoption assumptions, the pilot data will show you where the gap is before you are committed to 20 locations.
Cost per implementation tracked against budget in real time means any overages are visible before they compound. Contract terms that cap migration and support fees remove the cost categories most likely to grow after signature.
Schedule a call to see how Overjet structures the pilot financial model and what the per-practice numbers look like for DSOs at your scale.
Here's What CFOs Ask Us Most
How do we know the production uplift numbers are real and not vendor projections?
The pilot produces your own production-per-practice data from 3 to 5 of your locations before any rollout commitment. You are not approving a rollout based on Overjet's client averages. You are approving it based on measured outcomes from your own practices.
What happens to the TCO model if provider adoption is lower than projected?
Overjet tracks utilization daily and intervenes the same day adoption drops at a location. The adoption risk is managed in real time. If a location is underperforming on utilization, the issue is visible and corrected before it compounds across the quarter.
How do we handle support and migration costs as we add locations?
Contract terms cap migration and support fees. The cost categories most likely to grow after signature are fixed before you commit to scale. Per-location implementation cost is tracked against budget in real time during the pilot, so you have actuals before you model the full rollout.
What language do I use internally to justify the pilot investment before we have outcomes?
The pilot investment is approved to generate the financial data needed to make the rollout decision. Production per practice, adoption rates, and implementation cost against budget are measured at 3 to 5 locations. Rollout budget is contingent on those outcomes, not on vendor projections.
Why does FDA clearance matter to the financial model?
Overjet's 10 FDA clearances, more than any other dental AI company, give providers a clinical standard they can trust, which accelerates adoption. Faster adoption shortens the months-to-payback calculation and reduces the change-management cost in the TCO model.