The Gap Is Costing You More Than You Think
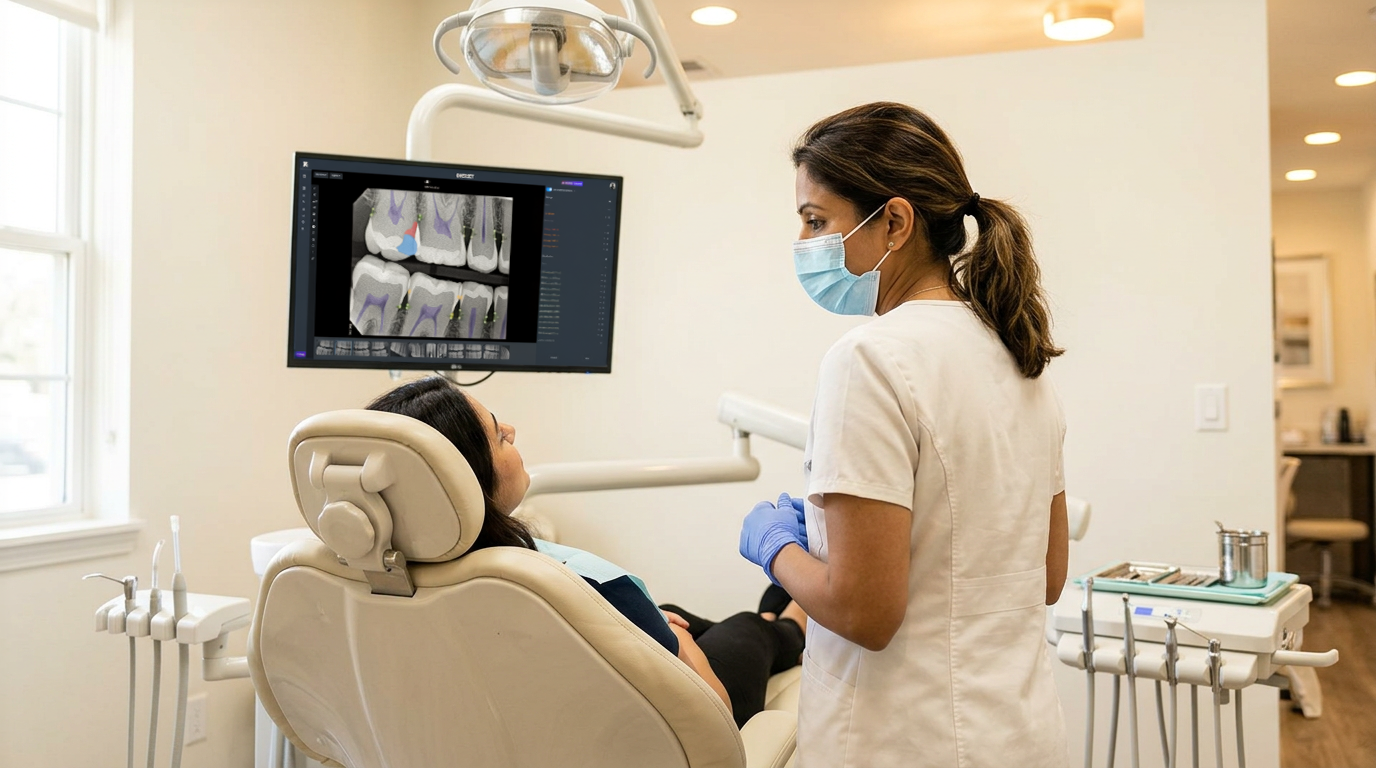
A hygienist at one location charts four perio cases per week. A hygienist at a comparable location charts one. The difference is the absence of a shared screening standard that travels with the clinician from location to location.
When documentation varies by hygienist, SRP approvals slow, insurance appeals accumulate, and hygiene production per hour becomes impossible to benchmark. You already have the data. The variance in perio case detection across your locations is the number that explains the production gap between your best and worst performers.
Why Perio Screening Variability Is a Revenue and Documentation Problem
Perio screening inconsistency suppresses hygiene production at every location where a case goes undetected. When a hygienist does not chart a finding, the SRP case does not exist in the revenue cycle. When documentation varies across locations, claims reviewers flag inconsistencies, appeals accumulate, and your hygienists absorb the rework that should never have been necessary.
The production gap between your highest and lowest performing hygiene locations is primarily a measurement problem. Without a shared screening standard, distinguishing between a location with a healthier patient population and a location where perio disease is going uncharted is difficult to spot. You can't benchmark what you can't measure consistently. You can only improve what you measure.
Standardized documentation makes it possible to track SRP case capture at the location level. When charting follows different standards across locations, you lose the ability to identify which offices are underperforming and why.
A Measurement Standard That Travels With the Patient Record
A phased SOP framework anchored to perio detection data makes standardization auditable without mandating identical clinical behavior at every location. A protocol that defines what gets measured and documented is not the same as a protocol that dictates the clinical decision. Treatment sequencing, patient communication, and case prioritization remain with the clinician. The measurement baseline becomes consistent.
Overjet is FDA-cleared for bone level quantification at 0.35mm precision, which means the measurement standard is a documented, defensible data point that travels with the patient record and holds up in a claims review. FDA clearance is the clinical foundation that makes perio screening data consistent enough to anchor a DSO-wide protocol.
The phased pilot rollout begins at three to five locations. Perio detection rates, SRP case capture, and documentation consistency are measured before full deployment. Hygienists adopt tools that reduce documentation time, and the adoption curve for this protocol is faster than any mandate-based rollout because the tool does not add steps. It replaces a subjective measurement with a documented one.
The Data Behind Consistent Perio Detection and Cleaner Claims
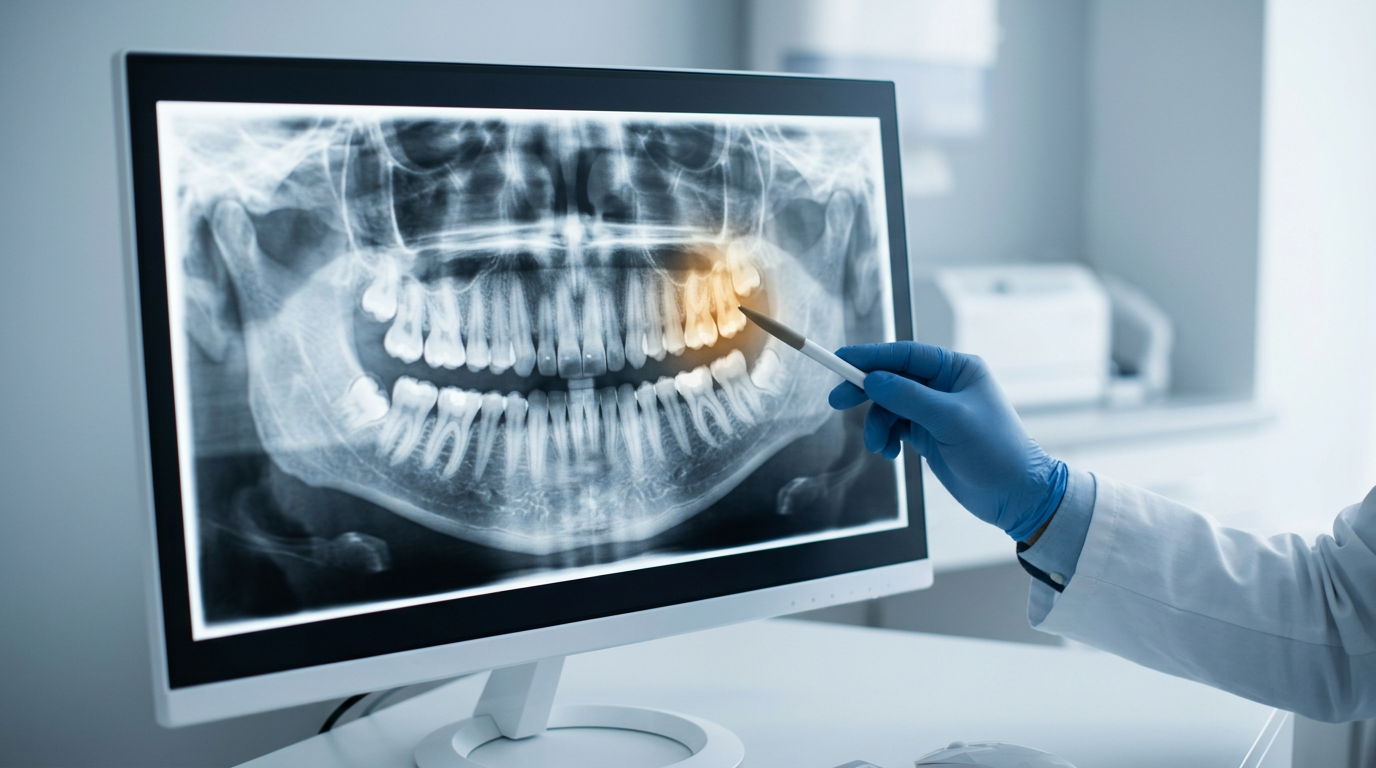
91% of dentists found more periodontal disease with AI-assisted screening. Perio cases that were previously going uncharted are now surfaced at the hygiene appointment, and each additional detected case that converts to SRP is direct hygiene revenue per location. Across a 50-location DSO, that compounds.
Claims decisions are 5x faster when perio charting follows a consistent documentation standard. Fewer appeals means less rework absorbed by your hygienists after the appointment, and faster claims decisions reduce the revenue cycle lag that erodes hygiene production metrics at the location level.
Treatment acceptance increases 15 to 25% when patients can see the pathology. Patients accept SRP when the finding is visible and documented. Higher acceptance per hygiene appointment lifts production per practice without adding chair time, and the documentation that supports acceptance also supports the claim.
Perio screening consistency is now measurable across all locations, and the data identifies which offices are below the DSO benchmark. That is the conversation that moves from clinical leadership to operational leadership.
What to Do With This Information
Schedule a call to see how Overjet's perio detection data maps to your current hygiene protocol and where the documentation gaps are costing you SRP revenue. The pilot model starts at three to five locations, measures perio case detection rates and SRP capture before full commitment, and gives you the per-location dollar impact before you scale.
Hygiene protocols are standardized and measurable across the DSO when the measurement standard is consistent. Production per practice includes hygiene revenue. Bring your COO into the conversation with location-level data that shows which offices are below benchmark and what closing that gap is worth.
Here's What Hygiene Leaders Ask Us Most
Does this work with our existing hygiene protocols, or does it require a new workflow?
Overjet integrates with your existing radiograph capture and charting workflow. Hygienists do not change how they take X-rays. The AI analyzes images already being captured and surfaces perio findings with documented measurements, which means the documentation step is faster, not additional.
How does FDA clearance affect how we can use this for perio screening and documentation?
Overjet's FDA clearance for bone level quantification means the measurement is a defensible clinical data point. Cleared technology for screening and documentation is the language your compliance team will ask for, and it is the language that holds up when a claim is reviewed or appealed.
What does perio case detection improvement look like in the first 30 days of a pilot?
Pilot locations typically see measurable increases in charted perio findings within the first month. The baseline comparison is your own historical detection rate at those locations. The data shows you whether the gap is in detection, documentation, or both, and it gives you a specific number to take to your COO.
How do I use this data to make the case internally for a DSO-wide rollout?
Perio screening consistency is now measurable across your pilot locations, and you can show which offices are below the DSO benchmark. SRP case capture by location, documentation consistency scores, and claims processing speed are the metrics that translate clinical performance into the production-per-practice language your COO tracks.