You already know which five locations are carrying your network and which five are dragging it down. That gap isn't random and it isn't a staffing problem. It's the predictable output of inconsistent clinical workflows, documentation standards, and diagnostic outputs compounding over time. Your standard is clear: one clinical workflow, one documentation standard, measured diagnostic consistency, applied everywhere. The problem isn't the standard. It's that every prior attempt to enforce it has either burned more regional management bandwidth than exists, triggered clinical resistance, or disrupted throughput more than it improved production.
The problem
The symptom is production variance. The root cause lives one layer deeper, in the imaging and documentation workflow every practice executes on every patient. It's assumed to be standardized. It usually isn't.
Different sensors. Different image enhancement settings. Different presentation habits. Different documentation outputs. These aren't clinical philosophy differences, they're workflow infrastructure gaps. And because they live at the point of care, they stay invisible to the ops layer until they surface as variance in a monthly report.
Inconsistent imaging drives inconsistent diagnostic outputs, which caps treatment acceptance, which caps production per practice. The 15 to 25% treatment acceptance lift associated with AI-powered visualization is the inverse proof: practices without consistent, AI-enhanced imaging are leaving measurable production on the table every day, in every operatory. You can't fix this by hiring more regional ops managers to manually enforce compliance. That path doesn't scale. The problem needs an infrastructure answer, not a headcount answer.
The standardization layer that moves production
The DSOs that have closed the gap between their top and bottom performers didn't do it by rewriting SOPs or adding field management layers. They standardized the one clinical layer every practice executes on every patient: imaging.
That's where Overjet comes in. Because it's FDA-cleared, it lets you stand behind this decision to implement it in front of your CFO, your clinical leadership, and your regional managers.
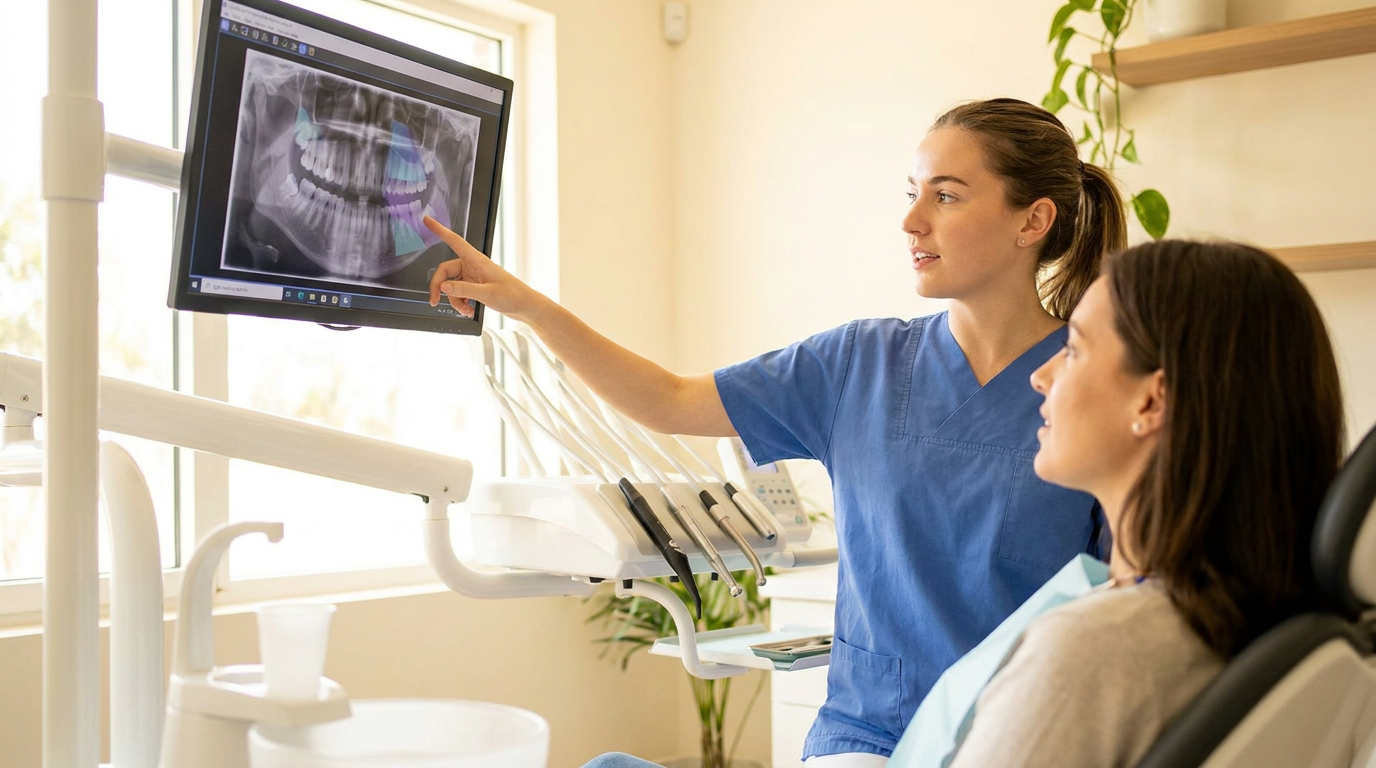
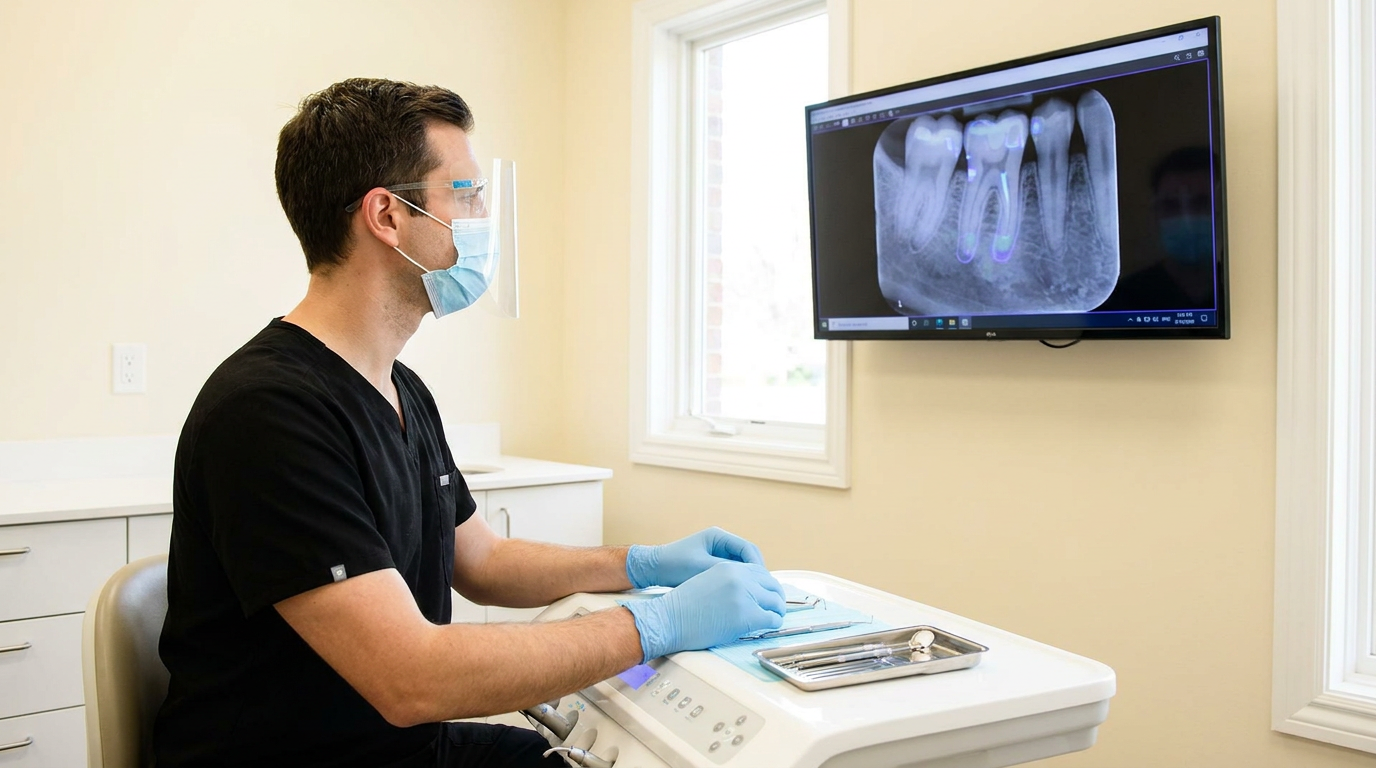
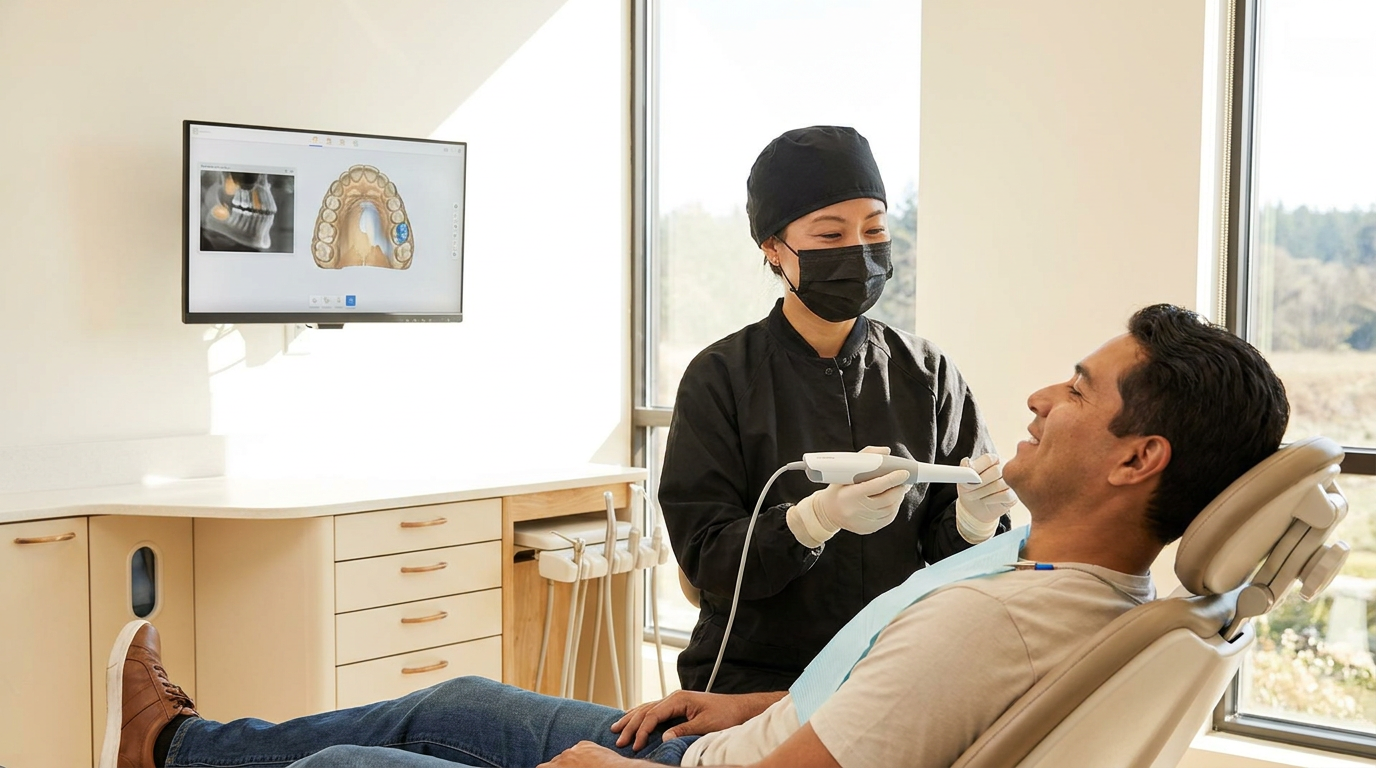
IRIS is dental imaging software with AI built in. It works with any sensor, intraoral camera, or pano machine already in your practices, so you're not replacing equipment or retraining staff on new hardware. You're replacing the software layer that governs how images are captured, enhanced, and presented, with AI annotations delivered at the point of capture, automatically, every time.
Standardization here doesn't mean eliminating clinical autonomy, and it's worth noting because your regional managers have probably already raised it. IRIS standardizes the workflow substrate (capture, annotation, documentation). Not what the dentist decides to treat. You control the workflow standard. The clinician keeps diagnostic autonomy. The standardization is invisible at the point of care, which is exactly what makes it scalable.
Proving ROI before full commitment
The pilot-first model is your proof mechanism: three to five locations, ROI proven before full deployment. You're measuring outcomes against a baseline, not evaluating vendor claims in isolation.
The accountability metric set before the pilot begins is 80% active utilization at 30 days. Not a lagging indicator reviewed at quarter-end. A live operational target with daily utilization tracking and same-day intervention when adoption drops. Most prior AI implementations in DSOs didn't fail because the diagnostic capability was insufficient. They failed because there was no adoption infrastructure. That's the structural fix.
The clinical proof connects directly to the production KPI. 100% of dentists found more caries with AI. 91% found more periodontal disease. Those are the upstream drivers of the 15 to 25% treatment acceptance lift and the 25% higher case acceptance that move production per practice. Dental groups using this model have achieved 10x average ROI, with implementation cost tracking (actual vs. projected) built in. You have a payback period to bring to your CFO before full rollout, not after.
For the VP of Operations running field execution, this translates into regional accountability structure: weekly utilization dashboards by region, adoption curve vs. projection tracking, and a defined blocker escalation path. Regional managers aren't absorbing a new change management burden. They're executing against a metric they can already see.
What this means for your network
The gap between your top and bottom performers isn't a permanent feature of running a multi-location DSO. It's a workflow infrastructure gap with a defined deployment cadence.
Book a demo to see the deployment model and utilization dashboard in practice.
What COOs ask us most
We've tried AI before and it didn't stick. What's different here?
Prior AI implementations in DSOs failed at the clinical adoption layer, not because the diagnostic capability was insufficient. IRIS is FDA-cleared dental imaging software with AI built in, not bolted on as a separate tool clinicians have to remember to use. Because it works with any existing sensor, IO camera, or pano machine, there is no hardware transition and no retraining on new equipment. The AI annotation appears automatically at the point of capture, every time, without requiring a behavior change from the clinician.
How do we prevent adoption from stalling mid-rollout, especially across regions where my managers don't have bandwidth for another initiative?
This is the question your VP of Operations is already asking. The deployment model includes daily utilization tracking with same-day intervention capability when adoption drops, not a weekly check-in after the damage is done. Regional managers receive weekly utilization dashboards by region, with adoption curve versus projection data and a defined blocker escalation path. The rollout is structured so regional managers are executing against a visible metric, not absorbing an open-ended change management responsibility. You set the 80 percent utilization target at 30 days; your VP of Operations executes against it with the tracking infrastructure already in place.
Do we have to replace our existing imaging equipment to standardize on one platform?
No. IRIS works with any sensor, IO camera, or pano machine already in your practices. You are replacing the software layer, not the hardware, which means there is no capital equipment spend, no equipment transition to manage, and no disruption to chair throughput during rollout. Standardization happens at the imaging software layer, which is what makes it deployable across a multi-location DSO without triggering the clinical resistance that typically accompanies equipment-level changes.