Periapical radiographs don't lie, but they do leave room for interpretation. A 0.5mm change at the crestal bone. A margin that looks slightly different from the last set of films. You're mid-appointment, the patient is in the chair, and you're making a judgment call on a finding that could easily get documented as monitor for the third visit in a row.
Bone loss assessment has a structural problem and in a busy DSO, it compounds quickly.
The Real Cost of a Deferred Read
When a borderline bone loss finding gets deferred, the immediate cost is invisible. The patient leaves without a treatment plan. The clinical note says watch and wait. Nobody catches the miss.
But the progression doesn't stop. By the time the finding becomes unambiguous, the window for less invasive treatment has often closed. The patient may need more extensive care than they would have six months earlier, and you're having a harder conversation without a clear visual record of how things changed.
At the individual provider level, this is a clinical quality problem. At the DSO level, it becomes a documentation problem, a consistency problem, and in some cases a legal exposure. When different providers across locations read the same finding differently, the inconsistency shows up in treatment patterns, claim denials, and patient outcomes.
What Overjet Vision AI Does
Overjet Vision AI is an FDA-cleared AI platform backed by 11 FDA clearances more than any other dental AI company. It analyzes existing periapical and bitewing radiographs and flags crestal and interproximal bone changes with millimeter-level precision. No new imaging hardware. No disruption to the current workflow.
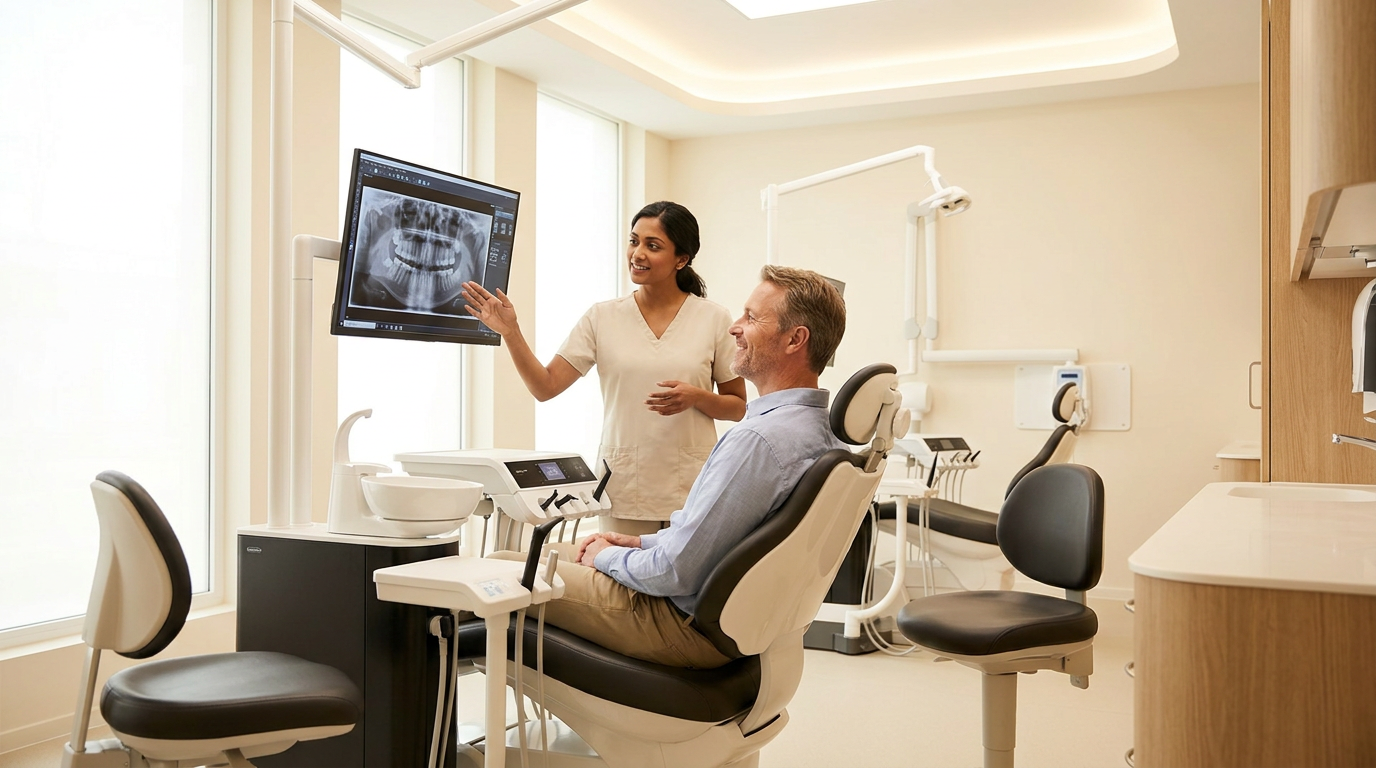
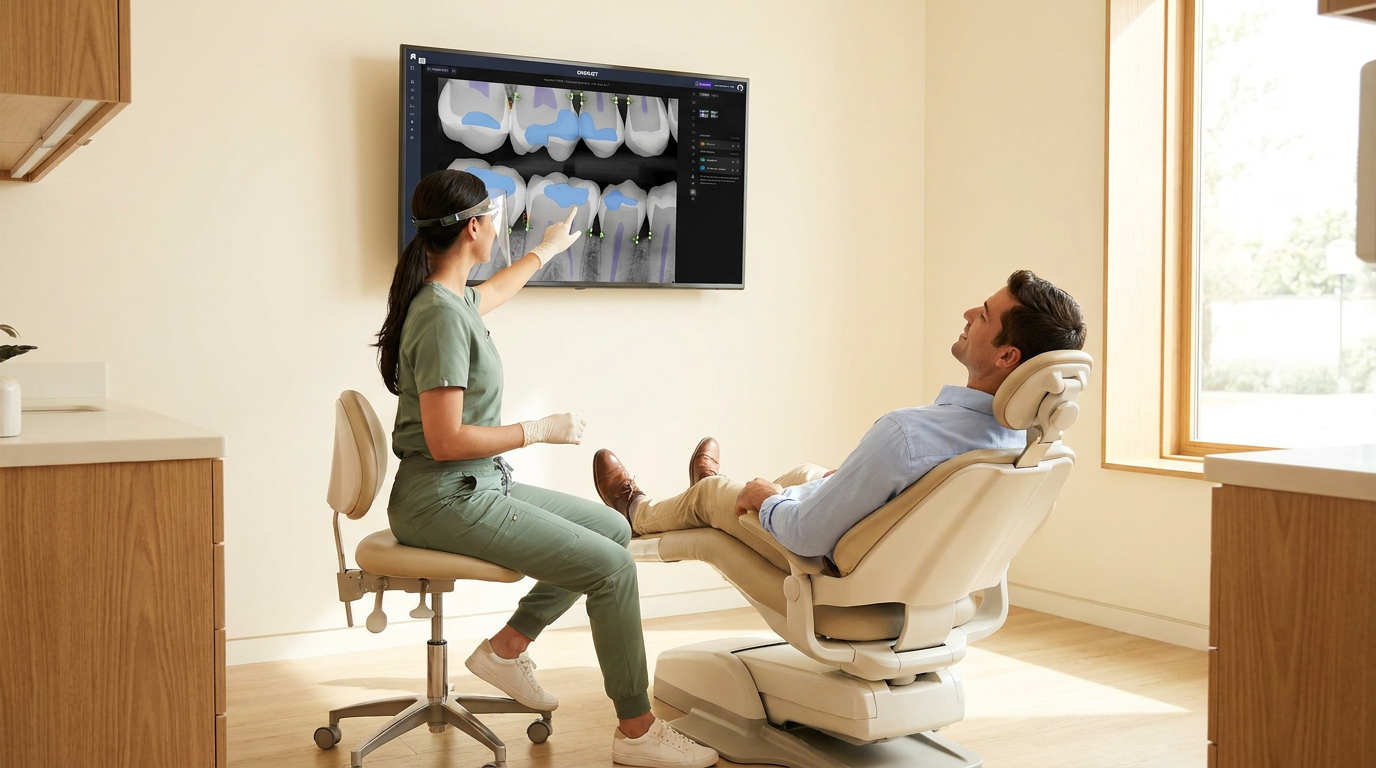
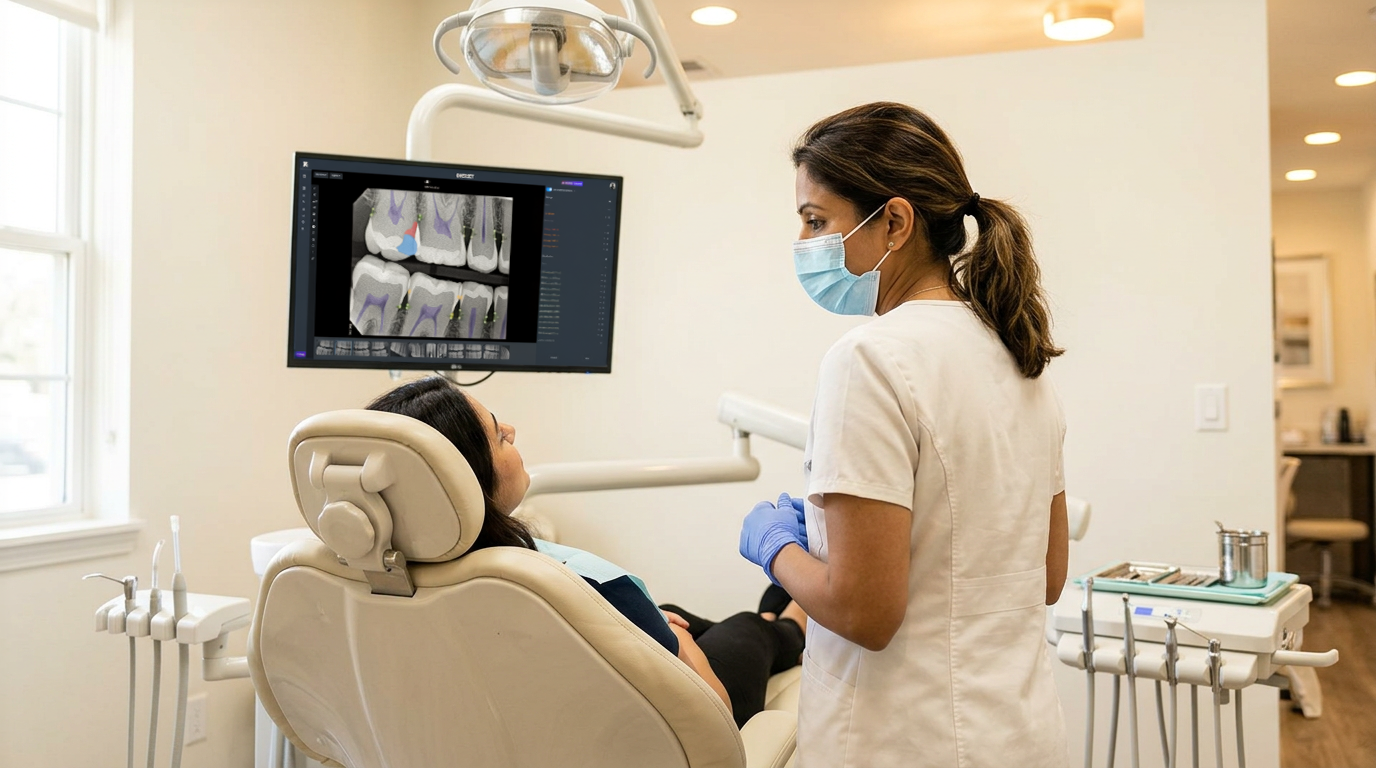
The output is not just an alert. Vision AI draws visual overlays directly onto the radiograph and delivers objective measurements. A dentist can see exactly where bone change has occurred and quantify it in the same motion. That shifts the diagnostic decision from a subjective read to one grounded in data.
For bone loss assessment specifically, this matters in two ways. First, subtle findings that might have been deferred now surface consistently, regardless of how full the schedule is or how experienced the provider. Second, those findings come with the kind of documentation that insurance reviewers, perio specialists, and risk managers can actually evaluate.
The FDA clinical studies behind Vision AI found that almost every general dentist was more accurate when using Overjet detecting decay and calculus with greater consistency than they did without AI assistance. Bone loss follows the same principle: objective measurements do not fluctuate with case volume, provider tenure, or end-of-day fatigue.
Where It Changes the Clinical Day
At the point of diagnosis, Vision AI shortens the gap between I think I am seeing something and a confident clinical decision. A dentist does not have to rely entirely on experience and eyeballing crestal levels. The AI surfaces the finding with measurement attached, so the next step is treatment planning, not second-guessing.
That confidence has a downstream effect on documentation. When an AI measurement backs up the clinical note, the record is defensible. It supports prior authorization, perio referrals, and if it ever comes to it, legal review. One board member from the Michigan Department of Licensing and Regulatory Affairs put it plainly: 80% of the malpractice cases I see over the year would have been dismissed if the doctor had good documentation.
At the patient conversation, a radiograph with the affected area outlined, measured, and visually annotated changes how patients receive a diagnosis. Patients say yes to treatment when they can see the evidence in their own mouth. Practices using Vision AI report a 25% increase in case acceptance.
The DSO Dimension
A single-location practice deals with one provider's diagnostic variability. A DSO deals with dozens or hundreds. That's a fundamentally different operational problem.
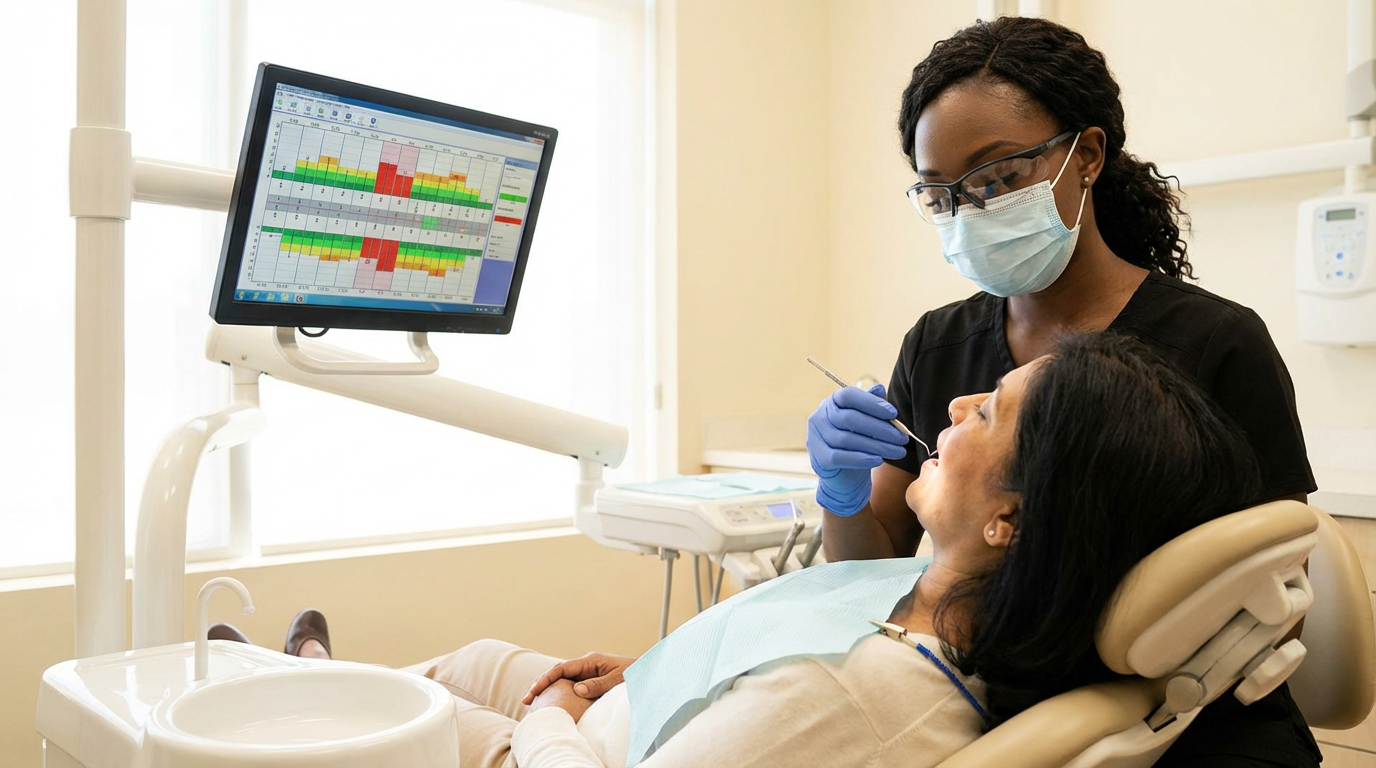
When every location runs Vision AI, the AI analysis is consistent regardless of who's holding the handpiece. A new associate and a 20-year veteran are working from the same objective measurements. That's what standardized clinical quality actually looks like not a policy document, but a consistent layer of intelligence applied to every image in every chair.
Dentists in DSO environments are measured on diagnosis accuracy, treatment acceptance, and chair-time efficiency. Vision AI improves the metrics that get reported, without adding documentation burden, because the AI output becomes part of the clinical record without extra charting steps.
For perio monitoring protocols specifically, Vision AI gives group practices a consistent, repeatable baseline. The same measurement standard across every patient, every provider, every location.
Ready to See It in Practice?
Less time deciding whether bone loss is present. More time having the treatment conversation with confidence. That's the shift Vision AI makes possible in a working DSO environment.
Book a Demo to see how Overjet Vision AI fits into your diagnostic workflow.
Frequently Asked Questions
Does Overjet Vision AI replace the dentist's clinical judgment?
No. Vision AI is an AI-assisted tool that gives clinicians objective data to inform their decisions, not to make decisions for them. The dentist reviews every finding and makes the final call. AI assists clinicians it does not replace them. The FDA clearances behind Vision AI are built on that principle.
Does Overjet Vision AI work with existing radiographs and imaging software?
Yes. Vision AI analyzes existing periapical and bitewing radiographs from your current imaging setup. No new hardware is required and there is no separate imaging workflow. It is designed to work within the systems DSOs already have in place.
What does the Overjet Vision AI output actually look like?
The AI overlays visual annotations directly onto the radiograph, outlining areas of bone change and attaching objective measurements. The dentist sees both the annotated image and the quantified data in the same view. That output can be used in the patient conversation, included in clinical documentation, and referenced for insurance or specialist referrals.
How do DSO dental teams use Overjet Vision AI in perio monitoring workflows?
Most teams integrate Vision AI as a consistent baseline measurement standard across patients and providers. Rather than relying on individual provider judgment to track crestal changes over time, the AI produces the same measurement methodology at every visit making it easier to identify progression between appointments, support perio referrals with objective data, and maintain documentation that holds up to insurance or clinical review.