Providers are leaving, and exit interviews point to the same two things: documentation burden and diagnostic uncertainty. Neither shows up on a wellness survey as a solvable problem, and neither gets fixed by a scheduling adjustment or a stipend. The CCO owns provider retention, and the levers available through HR don't reach the clinical workflow where the problem actually lives.
What's Driving Providers Out
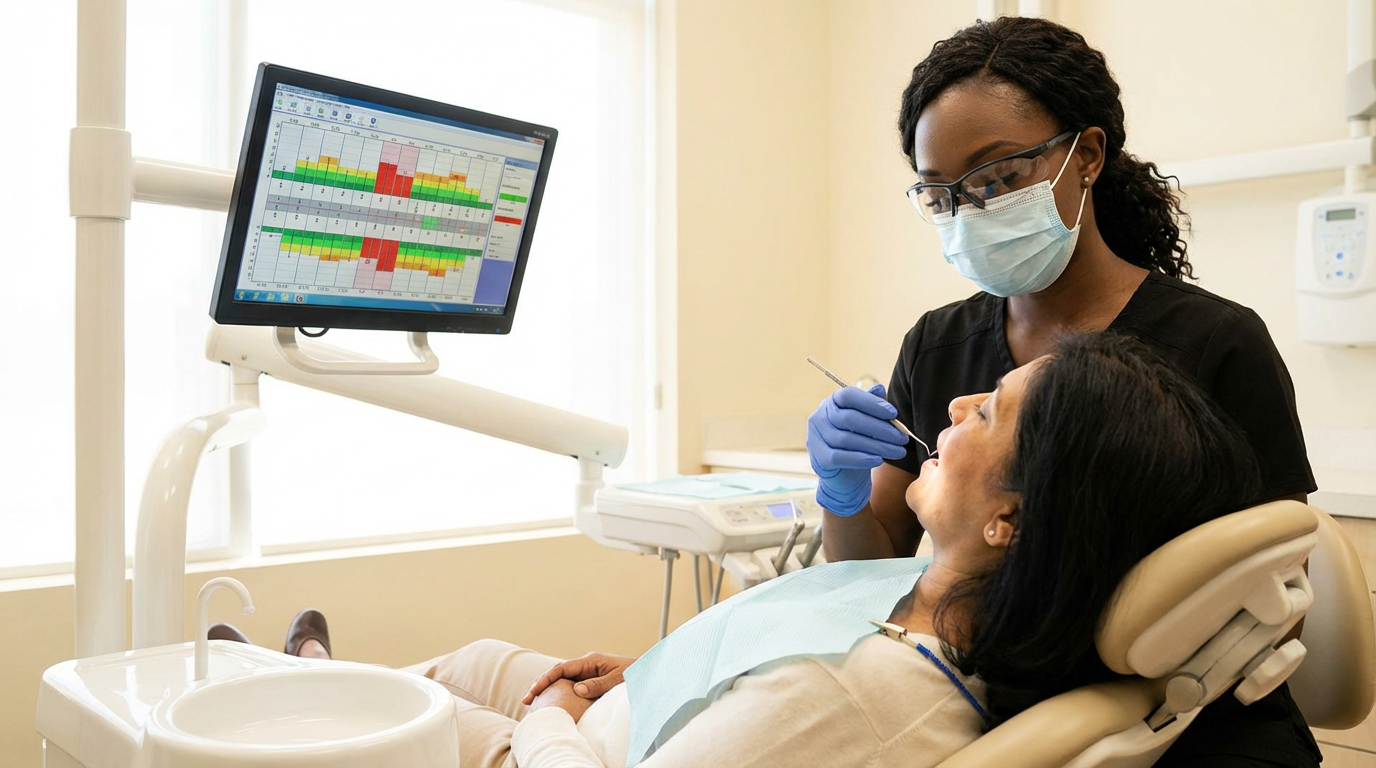
Documentation burden compounds across every patient encounter. A provider working across multiple locations encounters different charting standards at each one, no shared diagnostic baseline, and the expectation that they'll close their own notes after every appointment. That accumulation erodes clinical satisfaction over time.
Diagnostic inconsistency compounds the same way. A dentist without a consistent diagnostic standard carries the cognitive weight of every ambiguous radiograph. Perio screening inconsistency suppresses hygiene production at every location where a case goes undetected, and the provider absorbs the downstream friction when treatment plans are questioned or cases are missed. Providers who can't trust their own diagnostic baseline report lower clinical confidence, and lower clinical confidence accelerates the decision to leave.
Scheduling adjustments and wellness stipends don't reach this. The problem is embedded in the clinical workflow, and it needs a structural fix.
Preventing Burnout and Increasing Production
Burnout prevention built around documentation reduction and diagnostic standardization is also a production intervention. Providers who document faster see more patients. Providers with a consistent diagnostic baseline report higher clinical confidence. Both are measurable at the location level.
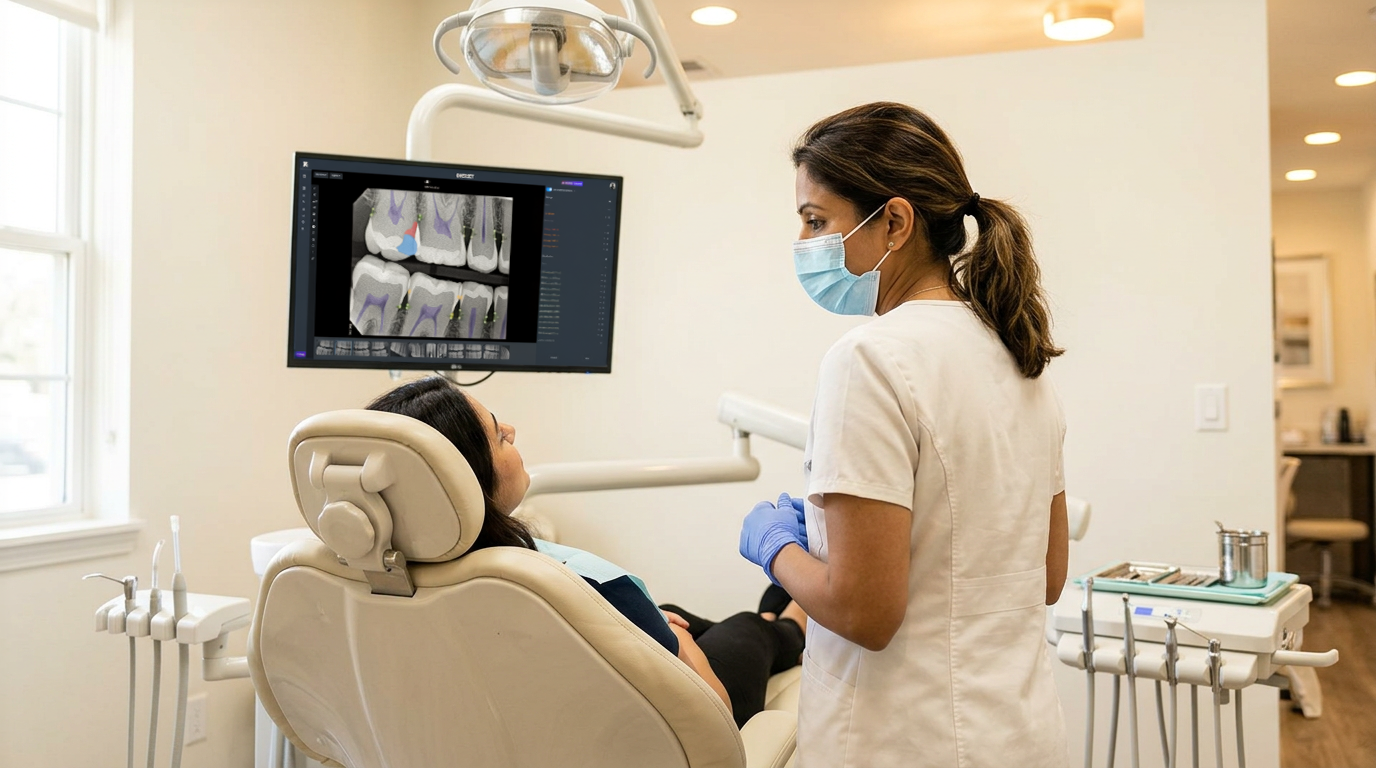
On the documentation side, Overjet Voice AI automates clinical notes as the provider speaks, eliminating post-appointment charting time. Documentation standardization happens across every location without manual enforcement. Providers focus on clinical care, and that's what reduces burnout at the practice level.
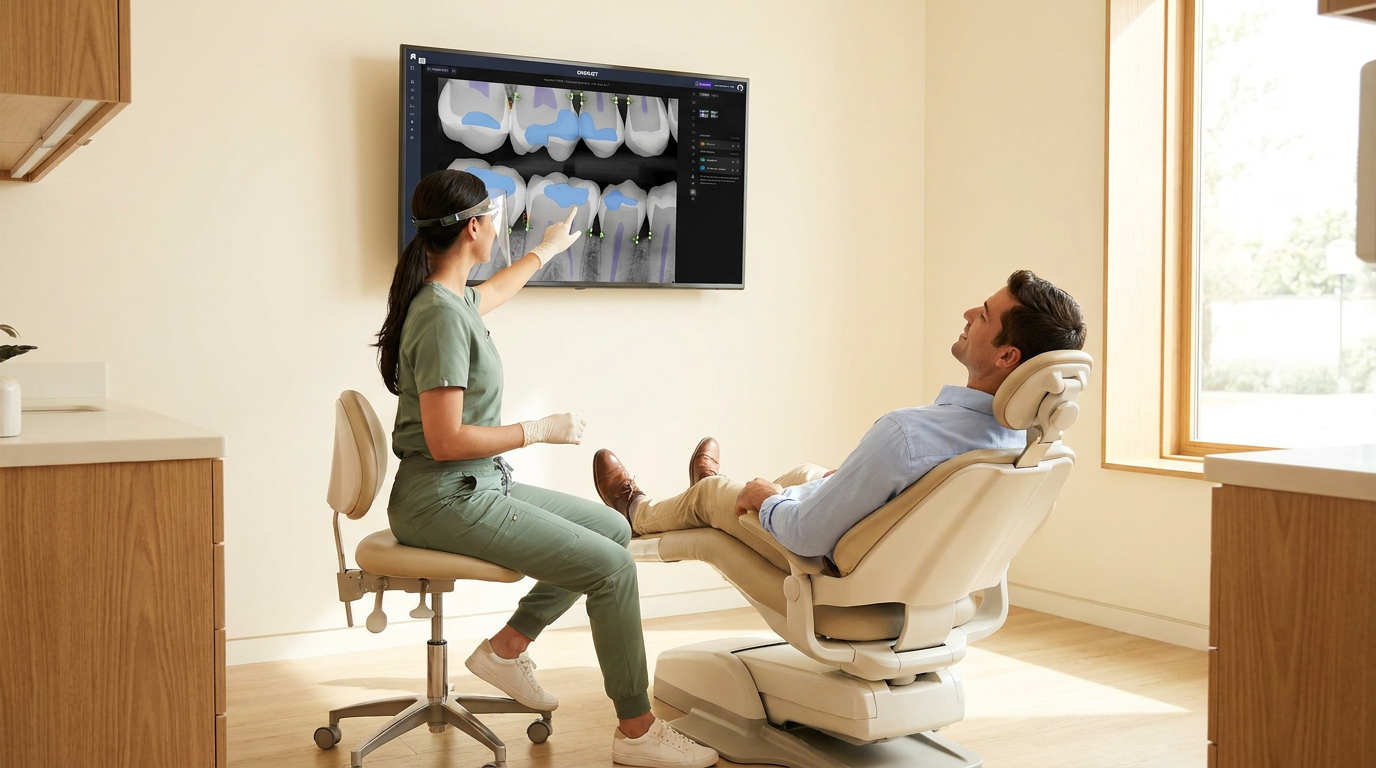
On the diagnostic side, Overjet Vision AI holds 10 FDA clearances, including caries detection and bone level quantification, more than any other dental AI company. Those clearances are the clinical credibility foundation that accelerates provider adoption, because dentists are working with a standard that has passed FDA scrutiny for the specific findings they document and bill. 100% of dentists found more caries with AI-assisted analysis, and 91% found more periodontal disease. Providers using this standard are practicing at a higher diagnostic level, which reduces the uncertainty that contributes to clinical dissatisfaction. Treatment acceptance increases 15 to 25%, and that gain is trackable by location.
Diagnostic Consistency Leads to Evidence-Based Coaching
Diagnostic consistency across all locations is now measurable, and that measurement makes provider coaching evidence-based rather than opinion-based. When a regional manager flags an underperforming office, the CCO has location-level data on diagnostic patterns, not anecdotal reports.
Overjet tracks utilization daily and intervenes the same day when adoption drops. Clinical adoption is monitored and supported rather than assumed, which means the CCO doesn't need to rely on regional managers manually auditing every office to confirm the standard is holding. An 80% active utilization target at 30 days post-rollout is achievable because the intervention mechanism is built into the platform.
Production per practice increases when providers are diagnosing consistently and documenting efficiently. The CCO sees higher quality diagnostics driving case acceptance. The VP of Operations sees a metric trackable by region. The underlying data supports both.
How to Reduce Provider Burnout
A pilot across three to five locations establishes ROI before any full deployment commitment. That structure gives the CCO clinical proof from live locations and gives the VP of Operations adoption data before a broader rollout is on the table.
Bring this to your VP of Operations as a clinical initiative with operational metrics attached. Standardized diagnostic protocol across the DSO is what this enables, and production per practice will increase because better diagnostics drive higher case acceptance. Flag any offices where adoption is stalling and use that data to drive the coaching conversation.
Schedule a call to learn more about how Overjet supports provider retention and diagnostic standardization across DSO locations.
Common Questions from CCOs
Will providers adopt this, or does it add friction to an already full clinical day?
Providers adopt it because it reduces work rather than adding it. Voice AI handles clinical notes as the provider speaks, and Vision AI's diagnostic analysis is embedded in the radiograph review they're already doing. The workflow change is subtractive.
How does FDA clearance change the clinical conversation with providers?
Overjet holds 10 FDA clearances, including caries detection and bone level quantification, more than any other dental AI company. Those clearances mean providers aren't being asked to trust a vendor's internal validation. The standard has passed FDA scrutiny for the specific findings they document and bill, and that removes the most common objection before it surfaces.
What language should I use when bringing this to my VP of Operations?
Frame it as a clinical initiative with trackable operational outcomes: standardized diagnostic protocol across all locations, documentation that doesn't require manual enforcement, and production per practice gains reportable by region. The utilization data is how you hold the rollout accountable.
How quickly does diagnostic consistency show up in the data after rollout?
Daily utilization tracking begins immediately, and location-level diagnostic patterns are visible within the first weeks of active use. The 80% utilization target at 30 days gives you a concrete milestone to evaluate before expanding to additional locations.
What does the pilot model look like?
Three to five locations run first. That structure lets you confirm ROI with real clinical and production data before committing to full deployment, and it gives your VP of Operations an adoption curve to reference when planning the broader rollout.