Your top locations aren't outperforming the rest because they have more providers. They're outperforming because they've accidentally solved a consistency problem you haven't been able to replicate at scale.
You can see exactly which locations are underperforming: the production-per-provider gaps, the operatory utilization numbers, the hygiene handoff breakdowns. The data isn't the problem. The problem is that fixing one location doesn't fix fifty. Every quarter, the answer from the field is the same: more staff, more hours, more chairs. And every quarter, the gap between your best and worst locations stays exactly where it was.
The Three Levers that Separate Top-Performing Locations
You've standardized the org chart, the scheduling templates, the hygiene protocols. And still, production per practice varies by 20 to 30 percent across locations with nearly identical headcount. The issue is diagnostic inconsistency, undertreated hygiene findings, and scheduling inefficiencies that compound silently across locations.
Three specific failure modes drive this gap.
First, providers at different locations are detecting and presenting the same conditions at different rates. The same patient gets a different treatment plan depending on which chair they sit in. That variability shows up directly in your production numbers.
Second, hygiene handoffs break down without a standardized workflow. The revenue that should follow a hygiene appointment doesn't, because the handoff between hygiene and restorative isn't a system: it's a habit that varies by location and by provider.
Third, operatory utilization drops when scheduling isn't built around actual chair capacity and provider tempo. Blocks go unfilled. High-value appointment types get scheduled inconsistently. The chair is available; the production isn't.
An Operational Playbook High-Performing DSOs Can Run Across Every Location
At 50-plus locations, the aggregate cost of these three failure modes is material. The DSOs closing the performance gap between their best and worst locations aren't doing it by hiring differently. They're doing it by standardizing the three levers that actually drive production per practice: scheduling and operatory utilization, clinical and hygiene workflow consistency, and case acceptance rates.
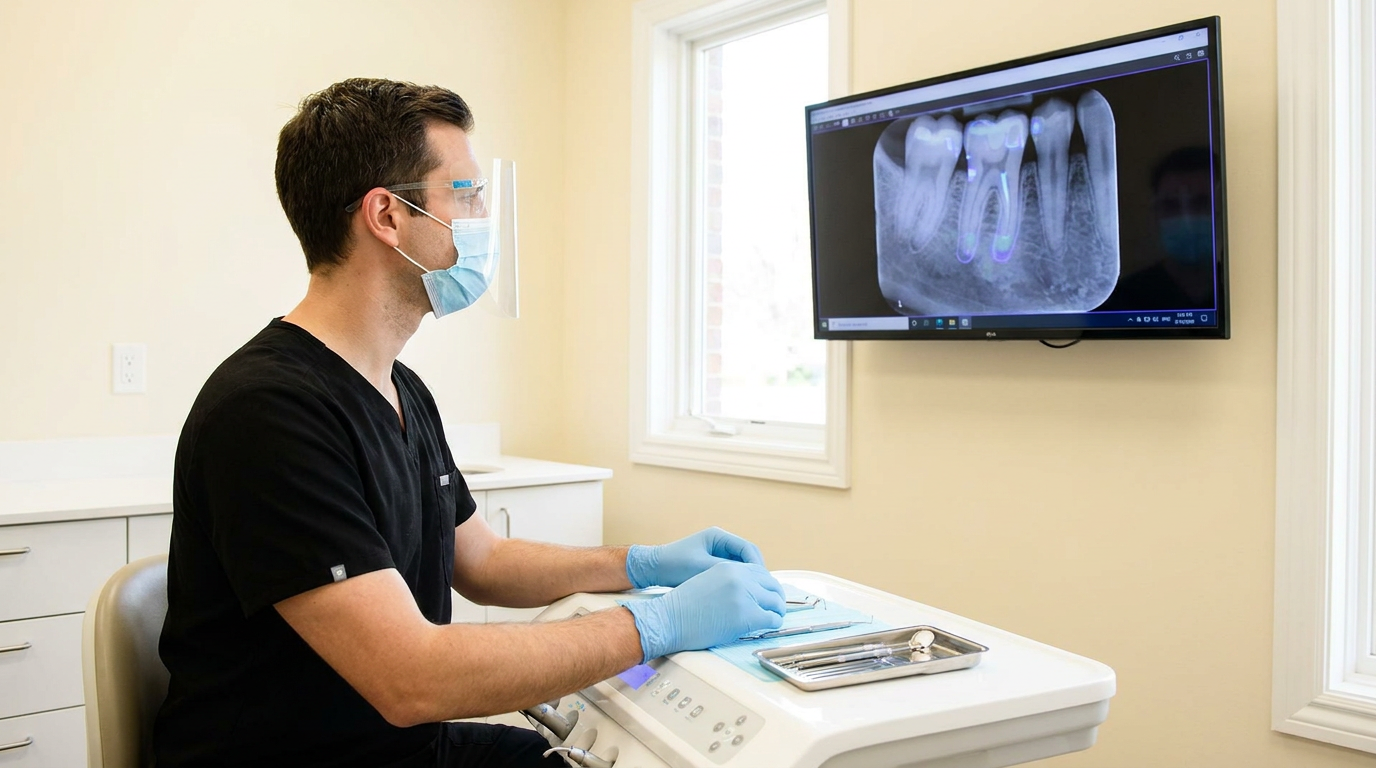
This is where Overjet fits. Overjet is FDA-cleared dental AI. It's a cleared diagnostic tool that can be built into clinical workflow without compliance exposure or provider resistance. FDA clearance is the foundation, not a feature checkbox.
Overjet is the measurement and consistency layer that makes the playbook replicable across locations. Here is what each lever looks like in operational terms.
Scheduling and operatory utilization. Most underperforming locations aren't underperforming because of provider headcount. They're running scheduling templates that were never built around actual chair capacity or provider tempo. Utilization rate and production per provider are the metrics that move here, and neither requires a PMS change.
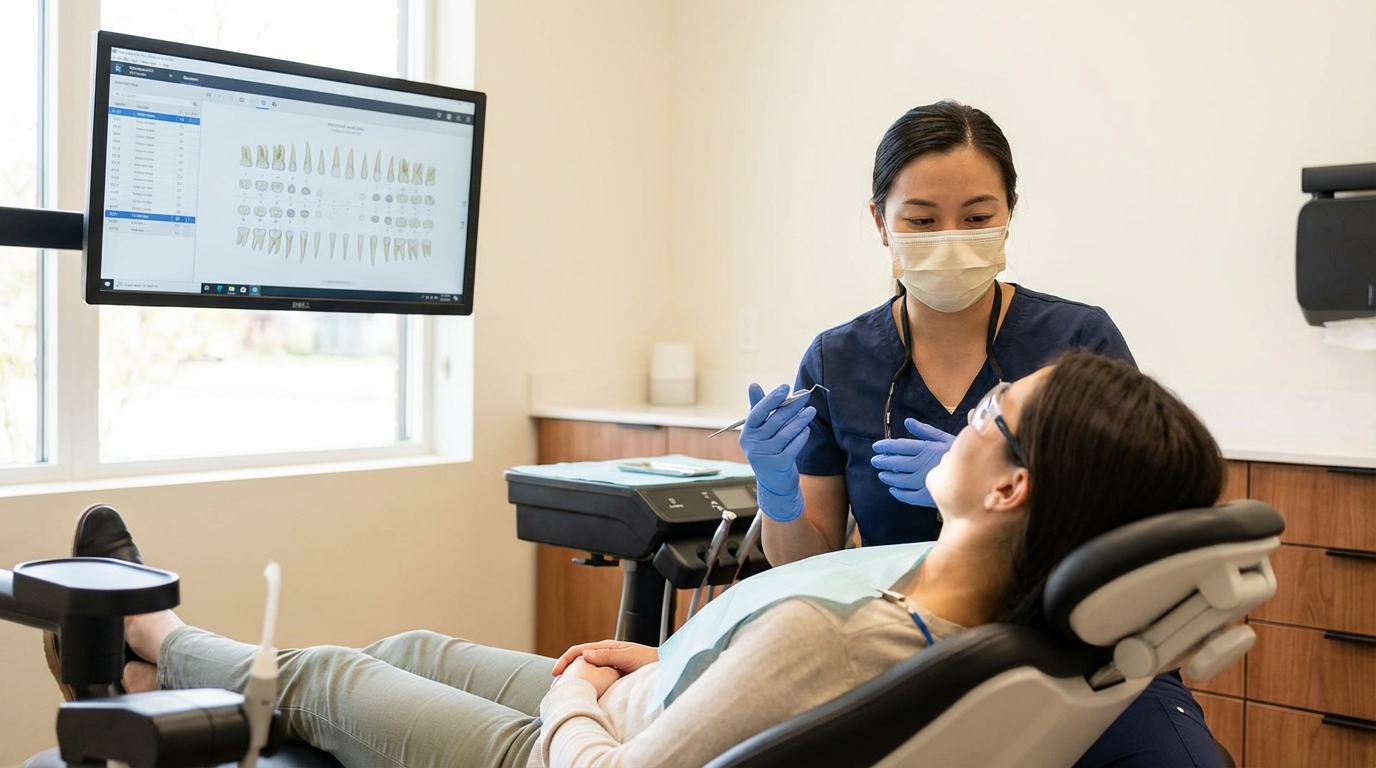
Clinical and hygiene workflow consistency. When providers have a consistent feedback loop tied to measurable detection data, diagnostic variability shrinks. The clinical encounter doesn't change. The consistency of what gets caught and documented does.
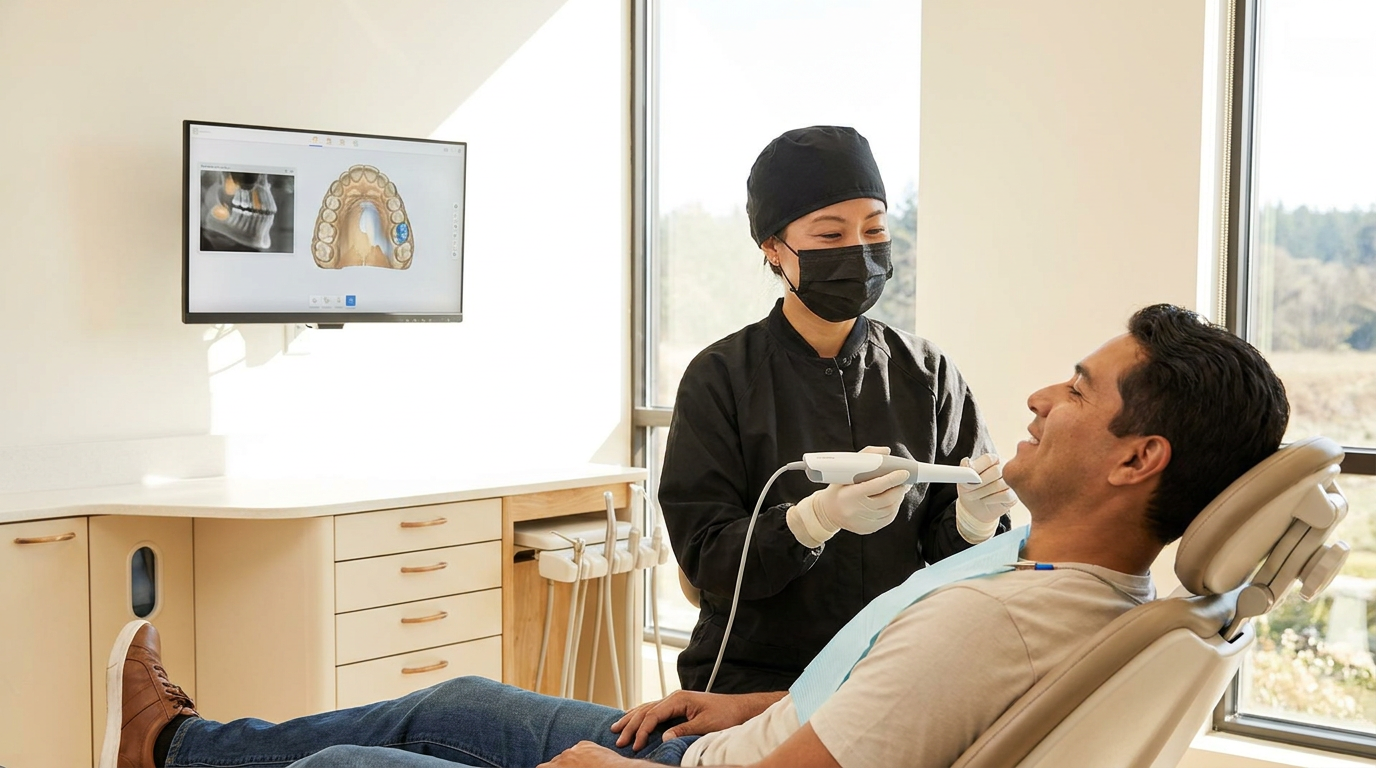
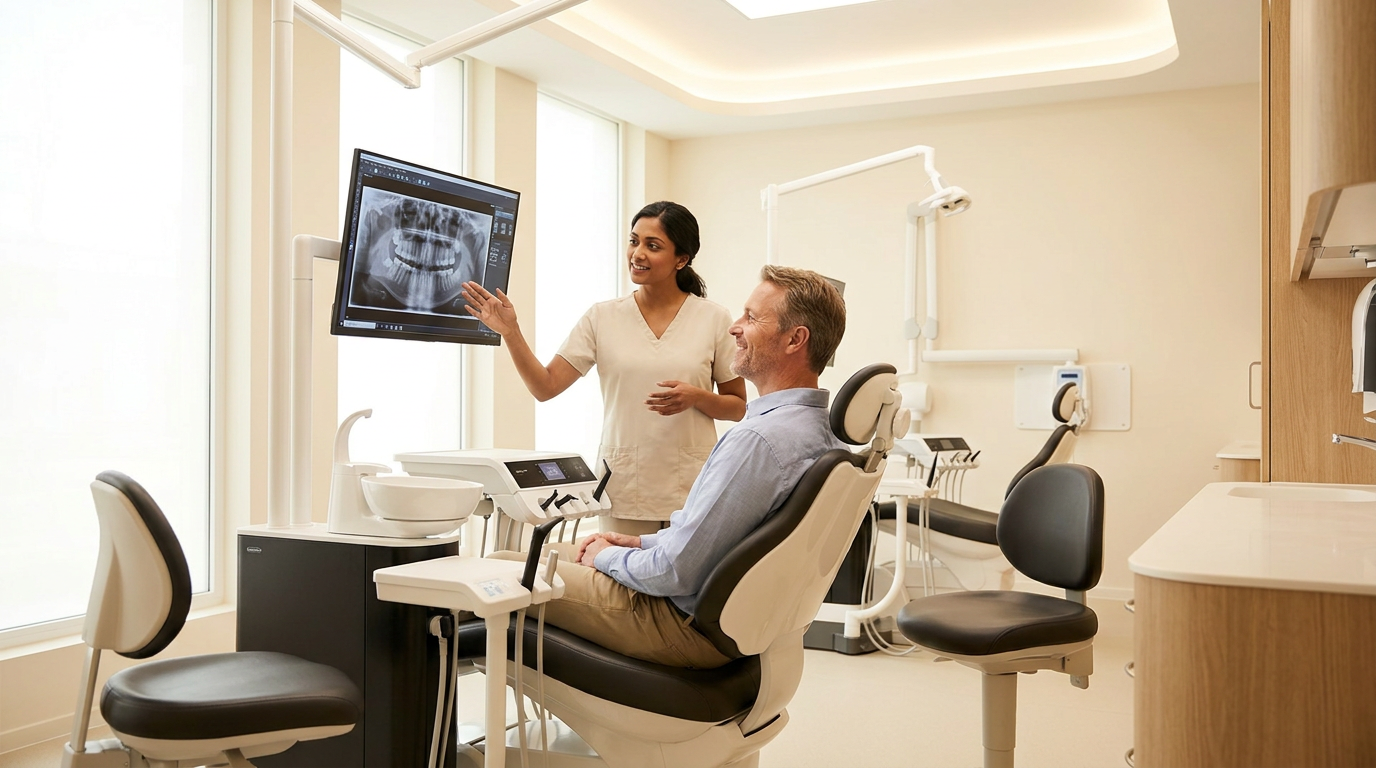
Case acceptance. AI-assisted visualization moves acceptance from a persuasion conversation to a visual one. Patients see their own diagnostic data. That changes the dynamic without changing the provider's role.
The Numbers Behind the Playbook, And What They Mean for Your Locations
100% of dentists found more caries with AI. 91% found more periodontal disease. If your providers are detecting conditions at different rates across locations, that variability is the production gap. It isn't a training problem. It's a detection consistency problem with a measurable solution.
On the case acceptance lever: AI-assisted visualization produces a 15 to 25 percent increase in treatment acceptance rates. A separate data point shows 25 percent higher case acceptance. For a COO evaluating repeatability, two independent data points on the same KPI signal that this isn't a one-location result. Both connect directly to average ticket and production per practice as the downstream metrics.
Dental groups running this playbook have seen 10x average ROI. The precision underlying the diagnostic consistency the playbook depends on is measurable: Overjet operates at 0.35mm accuracy, which means the detection consistency you're standardizing across locations is grounded in defensible, auditable data.
One additional metric for the CFO conversation: claims decisions run 5x faster, which broadens the ROI story into cash flow impact without requiring you to own the finance argument yourself.
The production per practice numbers above translate directly into per-location dollar impact. That calculation can be run against your own pilot data before any full deployment commitment is made.
Structure a Dental AI Pilot for your DSO
Production per practice is a utilization and consistency problem. There is a structured, three-lever playbook with measurable KPIs and a pilot-first model that lets you prove it in 3 to 5 locations before committing to full deployment.
The pilot-first model means you control the evaluation. Daily utilization tracking with same-day intervention when adoption drops means you're not betting on provider behavior: you're monitoring it in real time and correcting it before it becomes a sunk cost.
The next step isn't a product demo. It's a planning conversation: see what a 3 to 5 location pilot looks like before you commit to anything, or get the production benchmarks your CFO will ask for before you walk into that conversation.
A 3 to 5 location pilot gives you your own production data before any full deployment decision. That's the only number that matters to your CFO, and it's the only one that should matter to you.
Here's What COOs Ask Us Most
How do we know which of our locations has the most production upside before we start?
The starting point is a production-per-provider and operatory utilization audit across your location portfolio. Most DSOs find a 20 to 30 percent performance gap between their top and bottom quartile locations using data already in their PMS. The locations with the highest upside are typically those with strong scheduling volume but low case acceptance rates and undertreated hygiene findings, both of which are measurable before a single workflow change is made. A benchmarking conversation can help you identify which locations are the right pilot candidates.
We've tried to standardize clinical workflows before and it didn't stick. What makes this different?
Standardization without measurement doesn't hold. Providers revert to individual habits when there's no consistent feedback loop. The playbook works because each lever is tied to a KPI the location can see in real time: utilization rate, treatment acceptance rate, production per provider. When providers see diagnostic data alongside their own findings, adoption follows the evidence. One hundred percent of dentists found more caries with AI, and 91 percent found more periodontal disease. That's a detection consistency outcome that changes clinical behavior because the data is in the room.
What does the implementation timeline actually look like, and what does it require from my team?
The pilot runs 3 to 5 locations before any full deployment commitment is made. It layers into existing clinical workflow without a PMS replacement or a parallel documentation system. Daily utilization tracking is built into the pilot structure, with same-day intervention when adoption drops, so you're correcting rollout problems in real time rather than discovering them at the 90-day review. Implementation cost is tracked against budget throughout the pilot so you have actual-versus-projected spend data before you make a scale decision.
How do I make the ROI case to our CFO before we've run the pilot?
You don't need to make the full ROI case before the pilot. You need to make the case for the pilot. The pilot-first model is specifically designed so that the CFO's approval decision is based on your data, not vendor projections: production per practice uplift measured across your test locations, adoption rates tracked daily, and payback period calculated at actual adoption rates before full deployment is authorized. The numbers that exist before your pilot: dental groups running this playbook have seen 10x average ROI, and AI-assisted visualization produces a 15 to 25 percent increase in treatment acceptance rates.
What happens if provider adoption is low during the pilot?
Low adoption during the pilot is the exact variable the pilot is designed to surface and correct, not discover after the fact. Daily utilization tracking with same-day intervention means that if adoption drops at a pilot location, the response happens within 24 hours, not at the next quarterly review. You're not betting on provider behavior: you're monitoring it in real time and intervening before it becomes a sunk cost. If adoption doesn't reach the threshold that validates the ROI model, the pilot tells you that before you've committed to 50 locations.