Patients can understand their treatment completely and still say no. Here's what changes that.
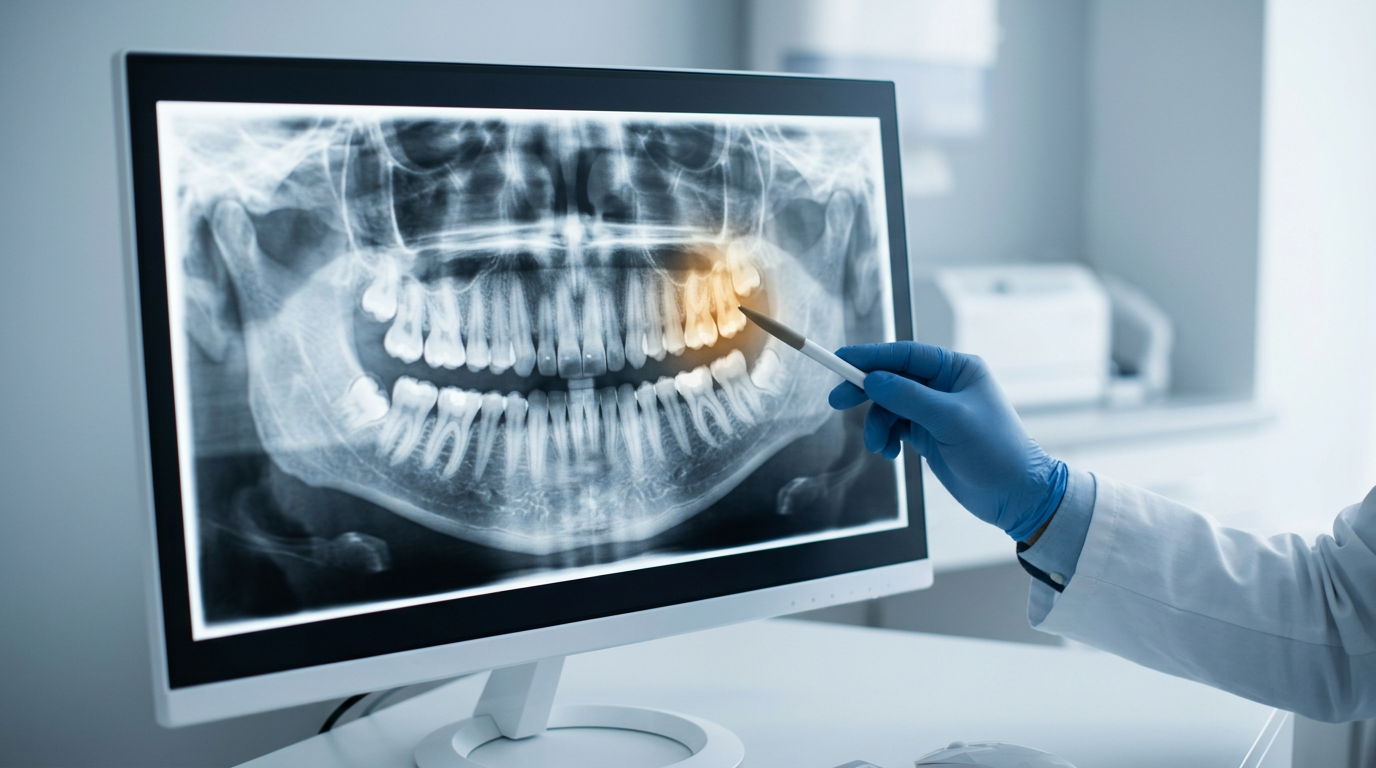
You found the cavity. You pulled up the X-ray, pointed to the finding, explained what it was and what it would become if left alone. The patient nodded. Asked a reasonable question or two. Said they'd think about it and call to schedule. Then they left.
That case sits in your unscheduled treatment queue now, next to three others from this week that went the same way. The clinical work was sound. The explanation was clear. And the patient still walked out without booking.
Patients don't decline because they distrust you. They decline because they can't see what you see, and invisible problems are easy to defer.
When Patients Can't See It, They Don't Believe It Needs to Happen Now
Patients accept what they can see and defer what they can't. This isn't a trust problem or a communication issue. It's a visibility problem. You're working with clinical information the patient has no frame of reference for. The X-ray means something to you. To them, it's a gray image with no obvious story.
Walk through what this costs in a single day. You have four or five explained-but-deferred cases. Each one is a patient who needed treatment and didn't schedule it. The production loss is real, but the more immediate problem is simpler: a patient left your chair without getting care they actually need.
There's a second cost. The verbal explanation is already taking time. You're spending two to three minutes per finding trying to close the gap between what you see and what the patient understands. That time adds up across every operatory and every appointment block, and it's not converting consistently. Longer explanations don't reliably change the outcome, and neither does more precise language.
The explanation itself isn't the variable. The approach is.
What the Practices With the Highest Case Acceptance Are Doing
The highest-accepting practices in DSO environments aren't using longer explanations or better scripts. They've replaced the verbal-only explanation with a structured visual walkthrough that runs 60 to 120 seconds and does the same job faster. When a patient can see the finding on their own X-ray, the explanation becomes self-evident. You're no longer asking them to trust a judgment call, because the image is doing the clinical work for you.
The framework is straightforward. Every walkthrough touches on three things: how the tooth feels now and later (comfort), what happens to it if treatment waits (longevity), and what the patient sees in the mirror (appearance). These aren't scripts. They're loose anchors the dentist narrates in their own voice, while the image does most of the explaining.
If patient education brings to mind a laminated brochure or a scripted speech, the concern about slowing things down is reasonable. But that's not what this is. It replaces the verbal-only explanation you're already giving, and it works faster.
Overjet's Vision AI is FDA-cleared for caries detection. That clearance matters at the chairside: when you show a patient the AI-annotated image on their X-ray, you're not offering an opinion, you're showing a clinically validated finding. The clearance is the foundation, and the annotated image is what makes the 60 to 120 second walkthrough work consistently, without asking your team to learn anything new.
The Numbers Behind What You're Already Seeing in the Operatory
Detection comes first. In studies, 100% of dentists found more caries using AI-assisted detection. Vision AI isn't just making existing findings easier to show; it's surfacing findings that would otherwise be missed. More to find means more cases on the schedule.
This isn't just about caries. Ninety-one percent of dentists found more periodontal disease with AI, which means Vision AI works across the full clinical picture. Precision runs to 0.35mm, a level of specificity that's hard to match on visual review alone.
And the acceptance outcome: practices using AI-assisted visualization see 15 to 25% higher treatment acceptance. Dentists report that it fits how they already work. They're not learning a new system; they're showing patients what they're already seeing, and letting the image do the work the verbal explanation was already trying to do. The appointment doesn't get longer, but the outcome improves.
The story for your ops team is simple. Production is up because you're catching more cases, and nothing about how you work has changed. That's the kind of evidence that moves internal conversations forward.
Schedule a Call
Patient education isn't a language problem. It's a visualization problem, and closing it doesn't require more time, a new system, or a different way of practicing.
Schedule a call to learn how Vision AI fits into your existing workflow, without adding time to your appointments or retraining your team.
The next patient in your chair doesn't have to leave without scheduling because they couldn't see what you saw. Two minutes of showing beats five minutes of explaining, every time.
Here's What Dentist Providers Ask Us Most
Is Vision AI actually FDA-cleared, or is that just marketing language?
Overjet's Vision AI is FDA-cleared for caries detection. The annotated findings on the X-ray are clinically validated, not the dentist's interpretation. At the chairside, that removes the burden of persuasion from the provider. The patient isn't being asked to trust a judgment call; they're looking at a cleared clinical finding.
Will I actually find more, or does it just make what I already see look better on screen?
In studies, 100% of dentists found more caries with AI-assisted detection, and 91% found more periodontal disease. Detection runs at 0.35mm precision, an accuracy that's hard to match on visual review alone. You're not just presenting more clearly; you're finding more to present in the first place.
How long does the patient walkthrough actually take?
The walkthrough runs 60 to 120 seconds. It replaces the verbal-only explanation that was already happening and usually taking longer. The appointment doesn't get extended, it just gets more effective.
If I want to bring this to my operations team, what's the adoption story I should be telling them?
Providers don't have to learn a new system. Vision AI surfaces findings on X-rays they're already taking, without retraining staff. Practices using AI-assisted visualization see 15 to 25% higher treatment acceptance, a metric ops teams can track, report on, and hold regional managers to. Rollout starts with 3 to 5 pilot locations to prove ROI before full deployment, and utilization is tracked daily, with same-day intervention if adoption drops. Your ops team has visibility and support from the start.
What does case acceptance actually look like after providers start using this?
Practices using AI-assisted visualization report 15 to 25% higher treatment acceptance. When patients can see the finding on their own X-ray, the decision to schedule accelerates. Dentists report that case acceptance improves without adding time per patient, because the visual is doing the work the verbal explanation was already trying to do.