You see the finding. Your patient sees a gray smear. What they can't see, they won't accept.
Your schedule is full. Between patients, you pull up a set of bitewings and make a judgment call in seconds. The image is low-contrast. The finding is early. You've done this thousands of times, and you're good at it. But the imaging technology you're reading hasn't changed much, and the diagnostic demand placed on it has only grown. The ambiguity isn't a skill gap. It's a visibility gap built into the workflow itself. And even when your read is right, the second half of the problem is waiting in the chair: your patient cannot see what you see, and what they cannot see, they will not pay for.
What You See and What Your Patient Believes
A full schedule means seconds per x-ray. You're reading bitewings between rooms, alone, with a patient already seated and a hygienist waiting on your next move. There's no second opinion available and no time to pull up a prior series for comparison. The problem you're facing is the imaging technology simply wasn't designed for the diagnostic volume a modern DSO practice demands.
Early caries and early perio findings are the hardest calls. A confident clinician still second-guesses them, and reasonably so. "Watch and wait" is sometimes the right clinical decision. But it's also the default when the finding is ambiguous and the schedule is full. The cost isn't only clinical. It's a deferred treatment conversation that may never happen, because the next visit brings a new set of pressures and the finding stays in the notes.
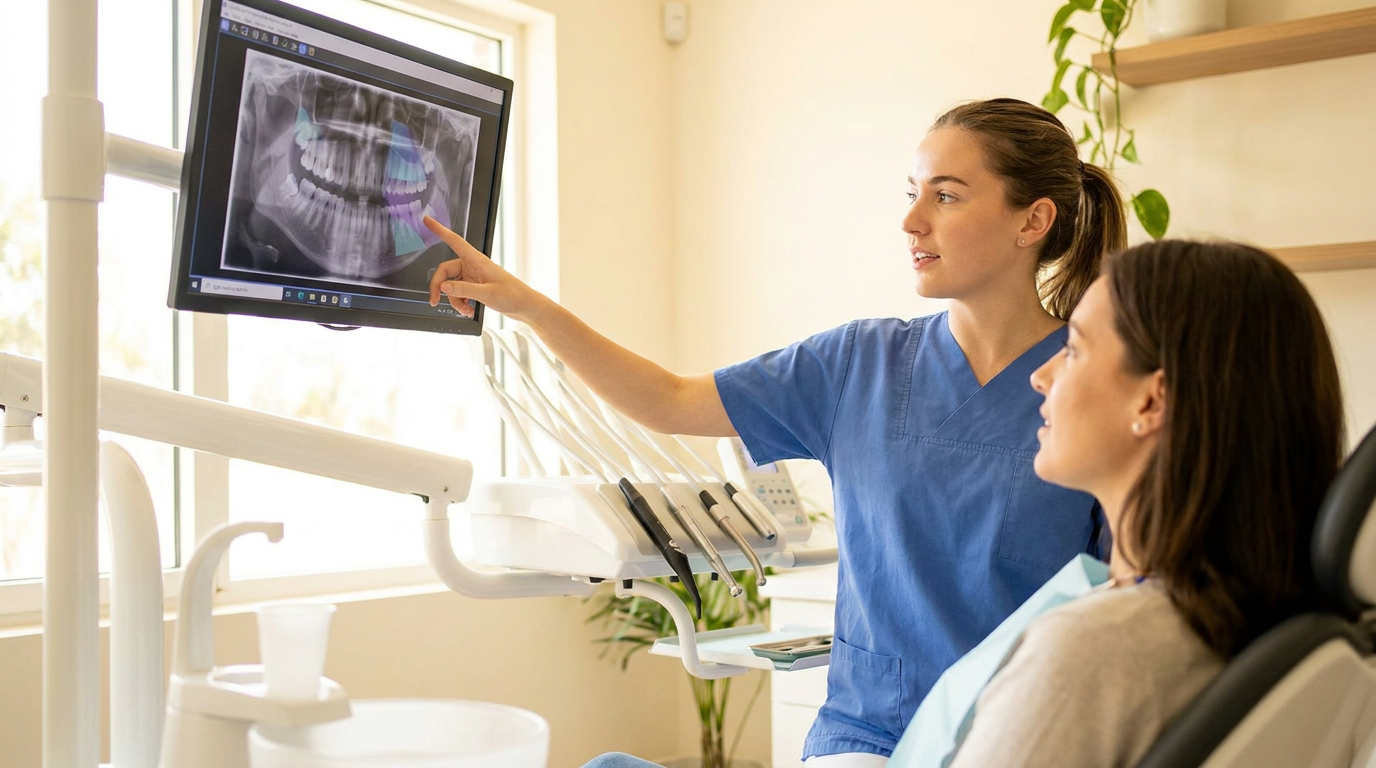
Then there's the chair-side moment. You point to the finding on the screen. The patient nods. You explain what you're seeing. They nod again. At the front desk, they decline. This isn't a sales problem. The patient genuinely couldn't see what you were pointing to, and without seeing it, they had no reason to act on it.
Every finding that doesn't translate into a treatment conversation is a patient who leaves without the care they need, and a schedule that doesn't reflect the work you actually did.
What AI-Assisted X-Ray Analysis Actually Does in Practice
The dental groups seeing the strongest case acceptance rates share one operational characteristic: the gap between what the clinician sees and what the patient understands has been closed, without adding a step to the clinical workflow. The mechanism is annotation, applied at the point of diagnosis, visible on the same screen where the x-ray already lives.
This is where Overjet Vision AI comes in. The foundation is FDA clearance, and it matters more than any feature description. Overjet Vision AI is FDA-cleared for both caries detection and bone level quantification. That clearance is the distinction between a regulated clinical tool and experimental software. This isn't an AI opinion layered on top of your read. It's a regulated output cleared by the FDA for the exact findings you're evaluating every day.
That distinction changes how you use it. The tool doesn't replace your judgment. It surfaces findings with clinical precision so you can act on them with confidence and show the patient exactly what was found and why treatment is indicated. The annotated image does the chair-side communication work that a gray smear on a monitor cannot. You remain the decision-maker. The annotation is the evidence you hand the patient before you leave the room.
The Evidence Behind the Confidence
In studies with practicing dentists, 100% found more caries with AI assistance, and 91% found more periodontal disease. These aren't indictments of clinical skill. They're detection amplifiers. The dentist who uses AI isn't being corrected. They're catching more, earlier, with less second-guessing on the calls that are hardest to make under schedule pressure.
Dentists who haven't used AI such as Overjet Vision AI, typically have three misconceptions.
"AI flags too much." Vision AI highlights findings. You decide what to do with them. A flagged finding that becomes a documented watch-and-wait decision is a clinical record, not a false positive that undermines your credibility.
"It'll slow me down." Vision AI overlays on your existing imaging software. There is no new platform to log into, no parallel system to manage, no retraining. The annotation appears where the x-ray already lives. You don't have to learn a new system. It helps you do what you're already doing.
"I don't trust AI for diagnosis." Vision AI has FDA clearance with 0.35mm precision in bone level measurement.
When using Vision AI, dentists see tangible improvement in the following areas.
Case acceptance: practices using AI-assisted visualization see a 15-25% increase in treatment acceptance. The annotated image is the mechanism. The dentist isn't selling harder. They're showing more clearly, and the patient is making an informed decision instead of a polite one. More accepted treatments means the schedule reflects the clinical work actually done.
Documentation: the annotated output is already captured, labeled, and exportable for insurance and billing. No new documentation step. The finding is recorded at the moment of diagnosis.
Adoption: Overjet uses a pilot-first model, deploying at 3-5 locations before any broader rollout. Results are measured before the decision to expand. The benchmark is 80% active utilization at 30 days, meaning the tool is being used in the majority of exams, not installed and ignored. Daily utilization tracking with same-day intervention when adoption drops means support exists if something isn't working. This isn't a tool that gets deployed and abandoned.
What's Next
AI dental x-ray software isn't a replacement for clinical judgment. It's the layer that makes clinical judgment visible, documentable, and persuasive enough to move a patient from "let's watch it" to "let's treat it." The dentist who uses it isn't practicing differently. They're practicing with more evidence behind every recommendation they were already making.
Schedule a call to see how Overjet fits into your current imaging workflow and what case acceptance looks like in practices your size.
Here's What Dentist Providers Ask Us Most
Is AI dental x-ray software actually FDA-cleared, or is that marketing language?
Overjet is FDA-cleared for both caries detection and bone level quantification, two of the most clinically significant findings in a standard x-ray read. FDA clearance means the tool has been evaluated against a regulatory standard for diagnostic accuracy, not simply marketed as AI-assisted. That distinction matters when you're the one signing off on the treatment recommendation.
Will this slow down my workflow or require me to learn a new system?
The tool overlays on your existing imaging software. There is no new platform to log into, no parallel system to manage, and no retraining required. The annotation appears where the x-ray already lives. The only change to your workflow is what you can show the patient before you leave the room.
What if AI flags findings I would have watched and waited on? Does that create liability?
AI highlights findings. You decide what to do with them. A flagged finding that becomes a documented watch-and-wait decision is a clinical record, not a liability. The tool's sensitivity is a feature: 100% of dentists found more caries with AI assistance, and 91% found more periodontal disease. Catching more earlier, with documentation, protects you and your patient.
How do practices measure whether this is actually driving results, and what does success look like at 30 days?
The benchmark used in DSO deployments is 80% active utilization at 30 days, meaning the tool is being used in the majority of exams, not just installed. Practices that hit that benchmark see a 15-25% increase in treatment acceptance, which shows up directly in production per practice. If your VP of Operations asks how the rollout is tracking, those are the two numbers that matter: utilization rate and case acceptance lift. Both are measurable within the first month.
What does the pilot process look like before a full DSO rollout?
Overjet deploys at 3-5 locations first. Results are measured, and the decision to expand is based on what actually happened, not a projection. You're not being asked to adopt something unproven. You're being asked to be part of the proof. Practices that complete the pilot have the data to tell the rest of the organization exactly what to expect.