Inconsistent perio screening has a measurable cost, and it shows up in your SRP numbers.
The same patient can leave one location with a perio diagnosis and another with a prophy. No amount of coaching has closed that gap permanently, and if you have been running a hygiene program across multiple locations for any length of time, you already know why. The problem is not the hygienists. The problem is the absence of a shared standard. Every hygienist is working from their own training, their own clinical judgment, and no common reference point. The goal has always been the same perio screening protocol across all locations, but every mechanism tried so far has created more work than it eliminates. This article shows what a different mechanism looks like.
Why the Absence of a Standard Leads to Inconsistency
A hygienist at Location A stages a patient at Stage II based on pocket depths and radiographic interpretation. The same patient visits Location B the following year and leaves with a prophy and a 'monitor' note. Neither hygienist is wrong by their own training. They have no shared reference point, so they each apply their own clinical judgment to the same clinical picture and arrive at different conclusions.
The downstream cost runs in three directions.
Perio cases go undetected. A patient who should be in an SRP cycle stays in a prophy cycle, and the disease progresses without intervention.
SRP revenue goes uncaptured. Cases that are never staged are cases that never convert to treatment.
Documentation gaps create audit exposure. When a claim is reviewed, a manually staged pocket chart without an objective clinical anchor does not hold up the way a documented, quantified finding does.
The coaching burden falls on hygiene leadership. You are solving a systems problem with a people solution, location by location, indefinitely. A new hygienist joins a location and the variation resets. A high-performing hygienist transfers and the standard travels with her, not with the protocol. The cost of leaving this unaddressed is current and measurable: a revenue gap and a compliance gap, not a future risk.
How High-Performing DSOs Built a Consistent Perio Detection Standard
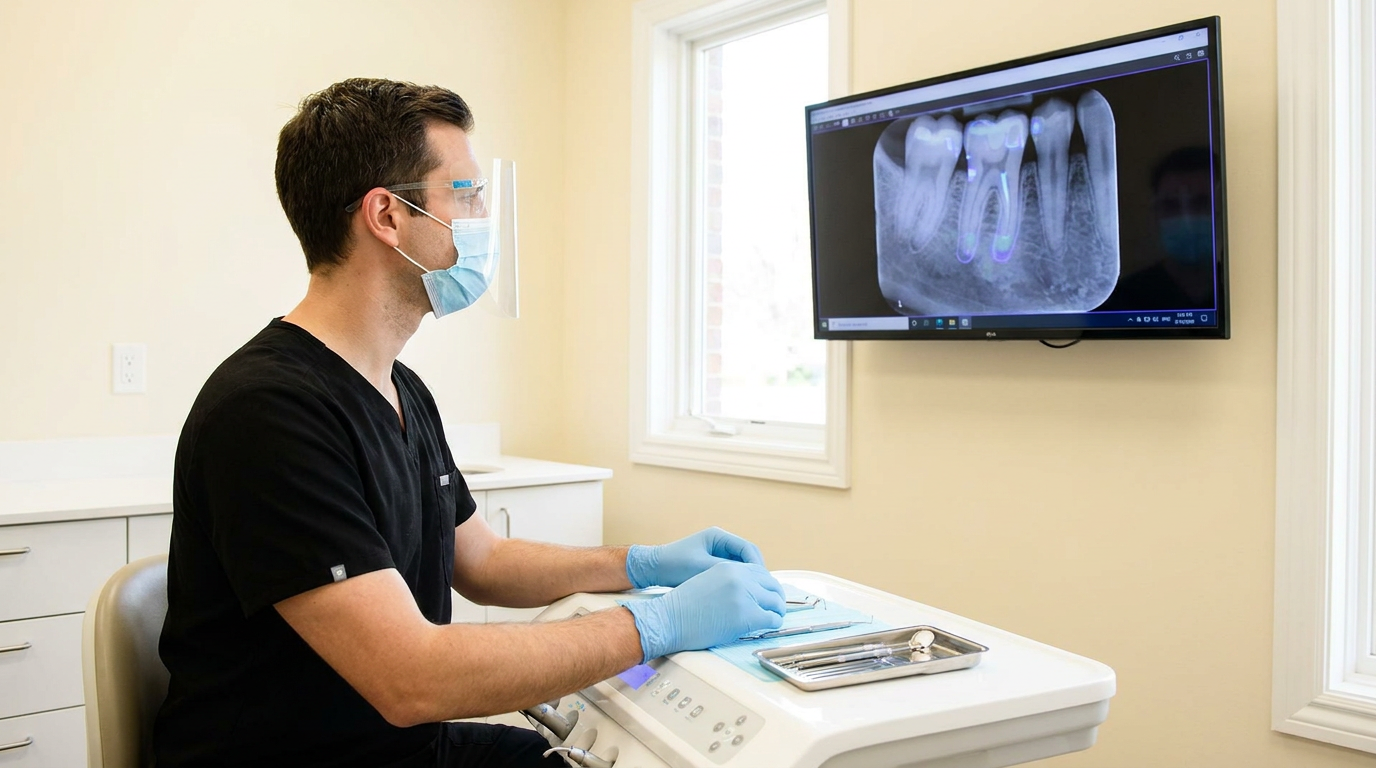
The DSOs with the strongest perio programs are not coaching harder. They have replaced subjective interpretation with an objective, location-agnostic detection layer that runs inside the existing workflow. This is not a new step in the hygiene appointment. It is a better reference point for the step that already exists: the radiograph review every hygienist is already conducting.
This is where Vision AI and Overjet enter. Overjet is the only AI company with FDA clearance for both caries detection and bone level quantification. FDA clearance is the reason a hygienist's perio finding, when surfaced through Overjet, is backed by cleared technology rather than an unvalidated algorithm. It holds up in a provider conversation, a claims review, or a compliance audit.
The clinical mechanism is bone level quantification at 0.35mm precision. Two hygienists at two different locations, working from the same AI-generated bone level reference point, are no longer producing two different staging outcomes on the same patient. The variation that coaching could not eliminate is structurally reduced because the reference point no longer varies by shift, location, or provider.
The consistent standard the hygiene program has been trying to build manually now has a mechanism.
The Evidence Behind AI Periodontal Disease Detection Software
Ninety-one percent of dentists found more periodontal disease when AI was part of the screening workflow. For a hygiene program, that number means the tool is not just documenting existing findings more neatly. It is catching disease that was previously missed, and it is doing so consistently across every location where it runs. Detection is the first gate. Consistency of detection is what makes the standard real.
The 0.35mm precision figure connects directly to documentation defensibility. A finding anchored in quantified bone level measurement holds up to a claims review in a way that a manually staged pocket chart does not. The hygienist is not making a soft call. She is surfacing a documented clinical signal backed by cleared technology.
The revenue connection runs through case acceptance. AI-assisted visualization of disease evidence drives 25% higher case acceptance. When patients can see the finding rather than only hear a staging number, they accept treatment at a higher rate. For hygiene program performance, that means more detected cases convert to accepted and completed SRP, which is the production metric that reflects the program's actual clinical output.
For conversations with operations or finance, Overjet delivers a 10x average ROI for dental groups. The hygiene leader is not the budget holder, but that number travels.
When dentists see that AI-assisted perio screening catches disease they would have missed, hygiene-sourced findings carry more weight. The 91% statistic comes from dentist behavior, not hygienist advocacy. That is why it lands in a provider conversation.
When the Standard Is in Place, Efficiency Follows
AI periodontal disease detection software is not a replacement for hygienist clinical judgment. It is the standardization layer that makes that judgment consistent, documentable, and defensible across every location. Hygienists are clinical gatekeepers for perio disease. Overjet Vision AI makes them better at it. The hygienist's diagnostic role becomes more defensible, because every finding is anchored in an objective reference point that travels with the protocol, not with the individual.
Schedule a call to learn more about how Overjet fits your hygiene program. The program that results looks like this: hygienists who catch more disease, document it faster, and walk into every provider conversation with data that holds up.
Here's What Hygiene Leaders Ask Us Most
Does AI periodontal disease detection software actually improve detection consistency across locations, or does it just add a documentation layer?
It improves detection first, and documentation consistency follows from that. When every hygienist at every location is working from the same AI-generated bone level reference point, staging variation by shift or provider is structurally reduced, not coached away. The documentation benefit is real, but it is a downstream outcome of better detection, not a substitute for it.
How accurate is AI-assisted perio screening compared to manual charting?
Overjet measures bone levels at 0.35mm precision, a level of specificity that exceeds unaided visual interpretation of radiographs. That precision is what makes the finding defensible: it is a quantified clinical signal backed by cleared technology, not a hygienist's estimate. For documentation and claims purposes, that distinction matters.
Will this slow down hygiene appointments or require hygienists to learn a new system?
The tool runs inside the existing workflow. It does not add a new step; it replaces the subjective interpretation step that already exists. Hygienists do not need to learn a new charting system. The AI surfaces findings during the radiograph review they are already conducting, and the net effect on chair time is neutral to positive, with faster documentation as a measurable outcome.
Our dentists are skeptical of AI-generated findings. How do we get provider buy-in without making it a mandate conversation?
Lead with the data dentists respond to: 91% of dentists found more periodontal disease when AI was part of the screening workflow. That statistic comes from dentist behavior, not hygiene advocacy. When a provider understands that AI-assisted perio screening catches disease they would have missed, the conversation shifts from whether to trust the tool to whether to trust the finding, and the finding is backed by FDA-cleared bone level quantification. The language that works in that conversation: Your hygienist is catching more perio cases. That is revenue for you and better outcomes for patients. The data is clinically validated, not a soft call.
How does better perio detection connect to SRP revenue and hygiene production numbers?
Detection is the first gate. You cannot capture SRP revenue from cases that are never staged. Once detection is consistent, the revenue connection runs through case acceptance: AI-assisted visualization of disease evidence drives 25% higher case acceptance, because patients who can see the finding accept treatment at a higher rate than patients who only hear a staging number. More detected cases convert to accepted and completed SRP, which is the production metric that reflects the program's actual clinical output.